Advancing Treatment Strategies for Better Outcomes in Diabetic Eye Disease
Diabetic retinopathy (DR) and diabetic macular edema (DME) present significant challenges for both patients and retina specialists. Patients often struggle with complex comorbidities, limited access to care, and maintaining consistent adherence to follow-up.1,2 First-generation anti-VEGF therapies, such as aflibercept 2 mg and ranibizumab, have been essential in managing retinal conditions; however, their injection burden and variable real-world outcomes have necessitated the development of second-generation agents.3,4 These newer, more advanced agents, including aflibercept 8 mg and faricimab, offer improved durability and potentially faster visual results.5,6 The following case studies from a recent closed panel discussion of both newly practicing and established retina specialists highlight their key insights that focus on practical clinical strategies for optimizing DR and DME management, including individual approaches to selecting appropriate therapies for real-world patients and extending their treatment.
— Priya S. Vakharia, MD
CASE 1: A PATIENT WITH CME WHO SWITCHED FROM AFLIBERCEPT 2 MG TO AFLIBERCEPT 8 MG
Esther Lee Kim, MD: Our first case is an affluent 79-year-old Caucasian female who was referred by her ophthalmologist for cystoid macular edema (CME) OU. She had been unresponsive to topical anti-inflammatory drops. Although she denied having diabetes, her records indicated type 2 diabetes since 2004. Her ocular history included monovision cataract surgery about 10 years prior, with her left eye corrected for near vision. Her presenting VA was 20/30 OD and 20/80 OS (pinhole 20/40 OS). No vitreous cells were observed on examination. An OCT showed foveal-involving CME OD with a central foveal thickness (CFT) of 427 μm and foveal-abutting CME OS with a CFT of 377 μm (Figure 1). Her general ophthalmologist prescribed topical steroid and nonsteroid anti-inflammatory (NSAID) drops then referred her to me. What is the next best step?
Arthi G. Venkat, MD, MS: I would differentiate between pseudophakic CME and DME using fluorescein angiography (FA). Optic disc leakage with macular involvement suggests Irvine-Gass syndrome or pseudophakic CME, whereas microaneurysms with edema indicate DME.7 This patient has a microaneurysm, indicating DME, so I would switch her to an anti-VEGF therapy.
David Chin Yee, MD, FASRS: Retinal exudates on OCT and during the exam also support a diabetes-related etiology rather than Irvine-Gass syndrome.8
Mohsin H. Ali, MD: I think her pathology is mainly from diabetes. But the right eye’s spatial distribution of edema suggests a small branch retinal vein occlusion (BRVO) may also be possible.
Dr. Kim: Comparing her FA from 2019 to 2023 revealed increased microaneurysms and leakage without the “hot disc,” effectively ruling out pseudophakic CME (Figure 2).
 Figure 1. Baseline OCT.
Figure 1. Baseline OCT.
 Figure 2. FA imaging.
Figure 2. FA imaging.
Dr. Venkat: Regarding treatment, many patients are more willing to use drops before injections. Initial improvement with drops often helps gain patient trust for further treatment.
Dr. Kim: I agree, trust is essential, especially for this patient who is in denial about her condition. Pushing for aggressive intervention may not be ideal here.
Tavish Nanda, MD: For my patients reluctant to accept their diagnosis, I obtain FA imaging as a valuable tool for visual demonstration, aiding in gaining patient acceptance.
Dr. Chin Yee: Importantly, if the patient’s vision is still relatively good, then continuing her topical drops and monitoring can help build confidence in the relationship with the referring clinician.
Dr. Kim: Our approach should also depend on the referring clinician’s stance—some are conservative while others prefer immediate intervention. Here, I opted to treat with aflibercept 2 mg based on the DRCR Network Protocol V, given her VA was worse than 20/25.9 Her dramatic treatment response confirmed the diabetic nature of her CME.
Ollya V. Fromal, MD: I would start with aflibercept 2 mg for patients with moderate-to-severe DME and a VA worse than 20/50, and with off-label intravitreal bevacizumab for treatment-naïve patients with mild DME and good vision.
Dr. Vakharia: Given treatment fatigue, how do you decide between aflibercept 2 mg and 8 mg?
Dr. Ali: I favor newer-generation branded medications overall. For this patient, I’d administer a second-generation agent, ie, aflibercept 8 mg, to treat her DME, considering that her OCT findings suggest she could extend her treatment interval to 8 weeks.10 Faricimab, another second-generation agent, is also a good option to treat her DME.11
Sruthi Arepalli, MD: I usually start with bevacizumab and switch to aflibercept 2 mg if needed, especially in settings like the Veterans Affairs hospital where payer constraints are less of an issue. If patients respond initially at 4 weeks but fail to extend, then I move to aflibercept 8 mg.
Dr. Kim: I also prefer branded drugs because I feel they maximize efficacy and durability from the get-go. This patient’s skepticism about the referral made it crucial to demonstrate rapid efficacy upfront. At the time of treatment, aflibercept 2 mg was the best option available, but this patient ultimately regressed when extending beyond 8 weeks. When aflibercept 8 mg became available, I promptly switched, enabling her to extend to a 12-week interval thus far and improving her VA to 20/25 OD and 20/60 OS (pinhole 20/30 OS).
CASE 2: EXTENDING DOSING INTERVALS IN A PATIENT WITH DME AND COMPLEX COMORBIDITIES
Dr. Chin Yee: Our second case is a 69-year-old female with new-onset DME in her left eye (Figure 3). She was treatment-naïve, and her VA was 20/50 OS. She had a 20-year history of diabetes, hyperlipidemia, heart disease, hypertension, and a body mass index (BMI) of 39. She was a smoker and used a scooter for mobility. Her fundus photos showed multiple hemorrhages, microaneurysms, and hard exudates. She is not your classic patient in a clinical trial, but a complex, real-world patient. I initiated intravitreal aflibercept 8 mg to hopefully achieve quick efficacy and to eventually extend the treatment interval.5 I usually avoid bevacizumab due to supply and dosing concerns.
 Figure 3. Baseline OCT.
Figure 3. Baseline OCT.
Dr. Venkat: I usually start with bevacizumab because of insurance restrictions, then I switch to aflibercept 2 mg, and move to aflibercept 8 mg later.
Dr. Chin Yee: In some cases, prior authorization allows us to start aflibercept 2 mg based on visual acuity. Medicare Fee-for-Service enables me to administer aflibercept 8 mg, offering fast results in my patients.
Dr. Vakharia: Let’s discuss who would start this patient on bevacizumab. Should we all start with bevacizumab to reduce health care costs? The 2-year results of the DRCR Protocol T clinical trial showed no difference in visual acuity outcomes between bevacizumab, aflibercept 2 mg, and ranibizumab at 2 years. The median number of injections was also the same between the three groups.12
Dr. Venkat: It’s debatable. While cheaper drugs may lower immediate costs, more injections over time may increase overall expenses. We need more studies to clarify this.
Dr. Nanda: One study, presented by Ella Leung, MD, at the American Society of Retina Specialists (ASRS) 2024 Annual meeting, suggested step-edit protocols cost more over time than allowing doctors to select a real-world treatment.13 For example, patients on bevacizumab may need more frequent visits than those initiated on a preferred agent. In addition, my patients on bevacizumab who miss follow-ups fall further behind in disease markers than those on aflibercept 8 mg.
Dr. Kim: Yes, real-world patients often miss follow-ups, unlike those in clinical trials. Multiple step-edits in therapy also make real-world outcomes differ from trial results.
Dr. Chin Yee: I agree. Real-world patients are more challenging than clinical trial participants. Durable agents that work faster can improve patient outcomes and reduce long-term costs, as seen in a 2023 cost analysis by the DRCR Network Protocol AC.14 The study by my colleague, Dr. Leung, confirmed that using branded medications can save costs by reducing treatment frequency.13
Dr. Vakharia: Why did you choose aflibercept 8 mg instead of faricimab?
Dr. Chin Yee: I’ve started some patients on faricimab, but I am now exploring aflibercept 8 mg for treatment-naïve patients. Unfortunately, there is no head-to-head study between aflibercept 8 mg and faricimab. Because of the availability of second-generation anti-VEGF therapies, I now use the dexamethasone intravitreal implant for DME less than before.15
Dr. Kim: Especially in younger, phakic patients, I’m using the dexamethasone implant as a third-line option, generally after newer anti-VEGF agents fail.
Leanne Clevenger, MD: I agree; I avoid the risk of inducing glaucoma in these patients.
Dr. Chin Yee: Back to this case, after one dose of aflibercept 8 mg, the patient’s visual acuity showed little improvement, but there was less retinal edema. Following the third dose (Figure 4), her edema and vision improved and as predicted, her hard exudates consolidated. At this point, would anyone consider extending her dosing interval to 7 or 8 weeks?
 Figure 4. OCT imaging after third dose of aflibercept 8 mg.
Figure 4. OCT imaging after third dose of aflibercept 8 mg.
Dr. Ali: I’m not optimistic that this patient will be able to extend to 8 weeks. I may attempt a single extension but would obtain a prior authorization for another drug in case the extension fails.
Dr. Kim: I would consider one extension to 7 weeks with aflibercept 8 mg in the case of DME but would have a low threshold to add a dexamethasone implant or switch to faricimab if I didn’t see further improvement at the next visit.
Hong-Uyen Hua, MD: I’m hesitant to extend this patient to 8 weeks, given that the decrease in edema is less drastic than I would have aimed for. I may be aggressive here and consider switching to faricimab.
Dr. Chin Yee: Given this patient’s reduction in CST, I did extend the dosing interval. If her retinal fluid had been worsening or no fluid change had occurred, then I would have reassessed her in 6 weeks and possibly switched agents. Obviously, this patient wouldn’t meet clinical trial criteria because of her comorbidities.5 I’ve treated many similar patients, and eventually we will see long-term results from these real-world patients. From my experience, I’ve observed that aflibercept 8 mg and faricimab take longer to see improvement in patients with diabetes compared to those with age-related macular degeneration (AMD).
Faricimab was another option for this patient, and I would’ve also extended with a 4-week interval. Before the availability of second-generation agents, we didn’t extend intervals this way. Is anyone routinely extending second-generation agents from 4 to 8 weeks or are you still extending by 2 weeks?
Dr. Venkat: When faricimab first launched, I tried extending by 4 weeks but reverted to standard treat-and-extend protocols. I still prefer small, 2-week extensions, particularly for AMD. I have more tolerance for fluid in DME, so I don’t follow a 2-week protocol as stringently
Dr. Ali: Extending by 4 weeks seems drastic; therefore, I typically extend by 1 to 2 weeks. During initial loading doses, I sometimes perform “mini extensions” of 4, 5, or 6 weeks to assess response and obtain a sense of whether they may be extended to 7 or 8 weeks later.
Dr. Vakharia: Of note, clinical trials often tolerate retinal fluid, whereas real-world doctors have varying comfort levels. The major trials for aflibercept 8 mg (PHOTON) and faricimab (YOSEMITE and RHINE) in DME had dose regimen modification criteria that tolerate retinal fluid and may extend patients by 4-week intervals.5,6 How do we reconcile tolerating retinal fluid in clinical trial patients who have noninferiority in vision with the tolerance of fluid in real-world patients? How much retinal fluid are you willing to tolerate? I’m curious to see what everyone would do. It’s fascinating that today’s retina specialists tolerate more fluid compared to 10 years ago when most retina specialists would’ve switched agents rather than extending intervals.
Dr. Venkat: Today’s physicians can be forced into tolerating fluid due to insurance protocols for dosing intervals. I’m not sure that tolerating more fluid as a community is for medical reasons.
Dr. Vakharia: In your opinion, what is currently the most challenging aspect of DME care?
Dr. Clevenger: I think it’s the complexity of diabetic patients, including comorbidities, access to care, and regular follow-ups. Newer, more durable agents may help alleviate these challenges.
Dr. Arepalli: Access to care and loss to follow-up are major issues. I often consider accelerating treatment with agents that allow for spacing out visits to reduce the disease impact of missed follow-ups.
Dr. Vakharia: For patients with DME, time is of the essence. We need to improve their vision as quickly as possible before they potentially disappear from care.
CASE 3: COMBINING ANTI-VEGF OR PRP IN A PATIENT WITH PDR
Dr. Chin Yee: My next case is a 62-year-old male with type 2 diabetes since 2006 and chronic kidney disease (CKD). He was working as a truck driver. He presented with proliferative diabetic retinopathy (PDR) characterized by a preretinal hemorrhage, significant edema, and retinal traction. His OCT image showed the hyaloid lifting off the fovea, indicating less chance of a tractional retinal detachment or vitreomacular traction and a better long-term prognosis of PDR. Unfortunately, we often see these patients too late. Why? Are we not emphasizing the need for routine diabetic eye exams effectively?
Dr. Nanda: PDR is often a silent disease. I see patients with severe tractional retinal detachments but with relatively good vision (ie, 20/30 to 20/40). When peripheral disease is overlooked, many referring providers may underestimate the severity, labeling disease as “moderate nonproliferative diabetic retinopathy (NPDR)” and advising yearly follow-up. Some patients with DR should be sent to a retina specialist sooner.
Dr. Kim: Diabetic eye disease progresses and improves slowly, making patient buy-in more challenging. Slow, subtle changes in vision often go unrecognized by patients, and the importance and urgency of treatment is not appreciated as well.
Dr. Fromal: Diabetic patients with severe kidney or peripheral arterial disease should automatically be flagged for eye exams. An electronic checklist or electronic medical record (EMR) pop-up could help. Education is key, especially in communities with socioeconomic challenges. Patients often hear about medications on television commercials, but there’s little messaging about diabetic eye exams.
Dr. Clevenger: I believe it’s currently unrealistic to screen every patient with kidney disease and diabetes. Future use of artificial intelligence (AI) and telehealth could play a vital role.
Dr. Venkat: I agree that emerging AI-based telehealth could help identify patients needing specialist care because not all eye care providers have equal training. I often receive referrals from optometrists for mild NPDR, only to find more severe disease.
Dr. Vakharia: This issue isn’t limited to optometrists; education gaps exist even among ophthalmologists. We need open communication among referring doctors without fear of losing the patient. We need to offer quick referrals for FA because wide-field FA often reveals hidden pathology. Overall, an effective system for returning patients to the referring doctor can build trust.
Dr. Chin Yee: To treat this patient, I offered aflibercept 8 mg because I am now focusing on the early treatment response with second-generation agents in treatment-naïve patients. Also, recent studies on PDR support starting with anti-VEGF therapy for DME followed by panretinal photocoagulation (PRP).16,17 I gave this patient four monthly injections because the first injection was a sample (Figure 5). In theory, after the fourth dose, I would extend the dosing interval to 8 weeks according to their OCT and visual acuity. What are your thoughts on extending the dosing interval, switching treatment, or adding PRP for this patient?
 Figure 5. OCT imaging from first through fourth anti-VEGF injection.
Figure 5. OCT imaging from first through fourth anti-VEGF injection.
Dr. Clevenger: I think this patient is at high risk for loss to follow-up because of their comorbidities. I would initiate a single session of PRP.
Dr. Arepalli: I agree that PRP seems appropriate given this patient’s risks and comorbidities. My struggle with patients with DME is deciding when to extend treatment. If we push for longer acting drugs to reduce fluid early, it’s tough to then justify accepting residual fluid later. I also want to avoid issues with visual outcomes in the future.
Dr. Ali: Importantly, we must consider this patient’s overall situation. As a truck driver, he needs to maintain 20/40 VA in both eyes. I wouldn’t extend his dosing intervals yet because of persistent fluid near the fovea. I’d keep 4-week dosing intervals and gradually introduce PRP in both eyes.
Dr. Venkat: I’m stricter about drying out the macula of patients with DME and a history of PRP. We aren’t only treating edema but also neovascularization. If we plan to treat with PRP, then we should aim to mitigate its load to potentially preserve the peripheral retina,18 especially for patients like truck drivers, and we should incorporate combination therapy. From day one, I tell patients, “If you want to protect your vision and livelihood, you don’t want me to obliterate your peripheral retina. We have to be strict about this.” Most patients listen.
Dr. Chin Yee: I agree. This patient understood the severity of his disease, and he has been extremely happy with his treatment interval and improvement in vision for his driving license requirements. Would anyone consider adding steroid therapy?
Dr. Vakharia: Absolutely, I add steroids quickly because I have low tolerance for fluid. I would also switch this patient to a different agent, like faricimab, for more flexibility. Did you switch him?
Dr. Chin Yee: No, he’s scheduled to return in 4 to 6 weeks for another sample of aflibercept 8 mg. But yes, if the edema doesn’t improve at that point, I may switch to faricimab.
Dr. Vakharia: What’s great about management of retinal disease is that we all approach it differently—there’s generally no right or wrong way to treat.
CASE 4: A MONOCULAR PATIENT WITH PDR TREATED WITH A DEXAMETHASONE IMPLANT
Dr. Vakharia: A 63-year-old female presented with a history of PDR and extensive PRP. Her VA was 20/200 OD and 20/80 OS. She worked as a nurse and was struggling with her vision for driving. Her FA imaging showed inactive PDR with leakage consistent with DME. In the right eye, there was disorganization of the retinal inner layers (DRIL) with possible macular ischemia. Additionally, OCT imaging suggested chronic edema (Figure 6). My main goal was to improve the vision in her left eye for driving, so I started her left eye on aflibercept 2 mg. How would you treat this patient?
Dr. Hua: If I weren’t limited by insurance, I’d go with aflibercept 8 mg or faricimab.
Dr. Kim: I’d consider adding steroid therapy after the second injection of aflibercept 2 mg because of the diffuse, spongy appearance of her edema and its likely chronic nature. I’d “throw the kitchen sink” at it.
Dr. Chin Yee: Subretinal fluid (SRF) is another biomarker I look for to use steroids. I typically administer combination therapy, especially with peripheral ischemic disease, to treat the VEGF load.
Dr. Ali: This patient has good PRP coverage, reducing her risk of conversion to PDR, and the DRIL in her right eye may suggest some potential benefit from steroid therapy. Also, her other eye likely lost vision due to untreated chronic CME, so “throwing the kitchen sink” at this patient is a good idea. In cases of active peripheral disease, like severe PDR, I usually prefer anti-VEGF therapy over steroids.
Dr. Vakharia: After I treated her with five aflibercept 2 mg injections, her VA improved to 20/50 OS, almost driving vision (Figure 7). Knowing this, how would you proceed?
 Figure 6. Baseline OCT imaging.
Figure 6. Baseline OCT imaging.
 Figure 7. OCT imaging after five intravitreal injections of anti-VEGF therapy.
Figure 7. OCT imaging after five intravitreal injections of anti-VEGF therapy.
Dr. Fromal: With the condition of her right eye, I would be more proactive. Adding steroid therapy could be beneficial. Depending on her response, I may consider faricimab later.
Dr. Nanda: Before switching, I’d try aflibercept 8 mg because she tolerated aflibercept 2 mg. If unsatisfied with the response, then I’d switch to faricimab.
Dr. Clevenger: Her response to anti-VEGF therapy wasn’t that effective. With the amount of fluid remaining, I’d add a steroid.
Dr. Vakharia: I agree, and I proceeded with a dexamethasone intravitreal implant. I find that patients with diabetes are “flight risks.” I typically load patients with only three injections then alter my course when needed. However, this patient was nervous about steroids, and I used the extra two injection procedures to have time to counsel her. She was pseudophakic, so cataract risk wasn’t an issue.
Dr. Venkat: I’d also consider a dexamethasone implant for her chronic edema to help flatten the retina,19 revealing how much outer retina remains. I would also alternate treatment with the dexamethasone implant and anti-VEGF therapy.
Dr. Vakharia: Now, 6 weeks after her dexamethasone implant, her VA is 20/40 and she can drive, but she still has edema. What is your next treatment approach?
Dr. Ali: I would switch to faricimab and continue with dexamethasone implants every 3 months.
Dr. Hua: I’d also switch to faricimab but consider a fluocinolone acetonide intravitreal implant for a long-acting effect.20,21
Dr. Vakharia: Twelve weeks after the first dexamethasone implant, I inserted her second implant. I did not administer combination therapy with anti-VEGF and intravitreal corticosteroid, although, I think that’s a fantastic idea. One month later, her VA improved to 20/32. She’s happy, although I am not because her retina is not fully dry. Believe it or not, she still has fluid so I observe her. Five months later, her edema returned, and her VA dropped to 20/40 (Figure 8). I administered another dexamethasone implant followed by a fluocinolone implant a month later. After this, her vision improved to 20/30 and her retina has only a small amount of residual IRF. The patient is happy. At future visits, I may consider redosing intravitreal steroids at the slightest hint of recurrent fluid or may consider combination therapy with intravitreal corticosteroid in combination with faricimab or aflibercept.
Dr. Chin Yee: With her being essentially monocular, I would have been more aggressive with combination therapy to get her retina as dry as possible. Still, it’s impressive how well she did despite some fluid.
Dr. Fromal: I also may have administered faricimab or aflibercept 8 mg in combination with steroids, but she responded well to steroids alone. This case demonstrates the art of retina treatment.
Dr. Vakharia: When observing these patients, especially those on intravitreal steroids, how often do you monitor them? What’s your approach to prevent loss to follow-up?
Dr. Arepalli: If patients have peripheral retinal disease, I prioritize treating with PRP to manage the risk of loss to follow-up. I also monitor patients with a history of PRP more frequently to catch any recurrence early, particularly patients with advanced disease.
 Figure 8. OCT imaging 5 months after second dexamethasone intravitreal implant.
Figure 8. OCT imaging 5 months after second dexamethasone intravitreal implant.
CASE 5: A 36-YEAR-OLD MALE WITH PDR AND RISK FACTORS FOR MAJOR COMPLICATIONS
Dr. Kim: Our next case is a 36-year-old Caucasian male who presented about 5 years ago with type 2 diabetes for 12 years, hypertension, and kidney disease. He experienced decreased vision for 2 to 3 months and saw his optometrist. His HbA1c was 7.6, and he was obese. His presenting VA was 20/40. His fundus photos showed neovascularization of the disc (NVD), neovascularization elsewhere (NVE), and scattered intraretinal hemorrhages in the macula and periphery. He also had signs of hypertensive retinopathy.
Concerningly, his FA revealed extensive areas of peripheral nonperfusion, indicating chronic disease and a high risk for future complications (Figure 9).22 It’s important to have a direct, extensive conversation with the patient regarding prognosis and educate them by showing them their retinal images. Clear explanations can greatly improve compliance.
Dr. Hua: This patient’s degree of PDR is alarming given his HbA1c. I’d investigate further, possibly with carotid ultrasounds or other tests, and find out whether he had uncontrolled diabetes in the past.
Dr. Kim: Great point, his past HbA1c was much higher, in the teens. The first two questions I always ask every patient with diabetes is “What was your last HbA1c? What’s been your highest HbA1c?”
I treated this patient with two monthly intravitreal injections of ranibizumab 0.3 mg and two sessions of PRP to minimize the number of anti-VEGF injections needed. After these two injections, his VA improved to 20/25 OD and 20/20 OS. His OCT images showed his ellipsoid zone was intact with no evidence of the biomarker DRIL.8 He had a phenomenal response. A critical point of this case is that this patient has been very compliant with follow-ups with his physicians. Did he have minimal background DR that quickly advanced? Is it possible for PDR to develop so quickly?
 Figure 9. Baseline FA imaging.
Figure 9. Baseline FA imaging.
Dr. Arepalli: Yes, rapid progression to PDR is possible, but it is also possible that this patient had silent or missed disease. Of note, his risk factors—obesity, diabetes duration, hypertension—made him a candidate for an early referral to a retina specialist for close observation. He requires more frequent follow-up than annually. There is always the possibility of silent eye disease with diabetes. I recommend an initial visit with a retina specialist for any patient with DR, then a follow-up visit at least every 3 to 6 months to avoid patients reaching end-stage retinal disease.
Dr. Ali: I think it’s highly unlikely he had no DR before. This retinopathy likely developed gradually over several years but was missed. Dilated fundus exams or proper interpretation of wide-field images may have caught it earlier.
Dr. Fromal: In general, can rapid progression of DR be caused by a sudden reduction in HbA1c from new diabetic drugs or during pregnancy?
Dr. Kim: Yes, both factors could cause rapid progression.23 Patients who rapidly lower their HbA1c often have a drastic worsening of their DR, similar to lowering blood pressure too quickly causing a stroke. I think the body needs more time to recalibrate. Points aside, severe NPDR has a 50% chance of progression to PDR within one year.24,25
Dr. Vakharia: I think this patient, who may be a “flight risk,” may benefit from the port delivery system (PDS) with ranibizumab if it is FDA approved for DME in the future. It’s a tough decision, especially with a young patient who could have the implant for decades.
Dr. Kim: Contrary to expectations, he’s been an exceptional patient, driving 2 hours for appointments despite his work schedule. Five years later, his vision is 20/20 in both eyes, and his case is a success story of timely intervention and faithful adherence to treatment (Figure 10).
Dr. Vakharia: This case demonstrates the importance of early referral and comprehensive care for patients with diabetes.
 Figure 10. Baseline OCT (A), final OCT 5 years later (B).
Figure 10. Baseline OCT (A), final OCT 5 years later (B).
CASE 6: A 20-YEAR-OLD MALE PILOT WITH PDR WHO REQUIRES FULL VISUAL FIELDS
Dr. Vakharia: This case involves a 20-year-old male pilot with type 1 diabetes who presented for a full exam. His VA was 20/25 OD and 20/20 OS. His OCT imaging had no retinal fluid, and FA imaging showed no NVE but areas of peripheral nonperfusion, classifying his disease as severe NPDR. He had an insulin pump, and his HbA1c was 6.9. However, he had a history of poor compliance.
At this visit, I chose to only monitor this patient. Two years later in 2017, he presented with PDR, indicated by neovascular fronds on fundus photos. His retina on OCT remained dry (Figure 11), but his FA showed significant NVE (Figure 12). Would anyone treat with anti-VEGF monotherapy or PRP now?
Dr. Hua: This is one of the rare instances in which I’d consider anti-VEGF monotherapy. Because he’s a pilot, it is critical for licensing requirements to preserve his peripheral vision by avoiding PRP therapy.18 His HbA1c is controlled, so anti-VEGF therapy may be his best option to avoid negatively affecting his career.
 Figure 11. OCT imaging in 2017 at time of PDR diagnosis.
Figure 11. OCT imaging in 2017 at time of PDR diagnosis.
 Figure 12. Baseline FA imaging in 2017 before treatment.
Figure 12. Baseline FA imaging in 2017 before treatment.
Dr. Vakharia: That is correct, regulations by the Federal Aviation Administration (FAA) require pilots to have 20/20 corrected distance VA and full visual fields, typically using Humphrey visual fields.26
In most cases of PDR, I do not choose anti-VEGF therapy alone because of the risk of loss to follow-up, but I made an exception this time. I started this patient on bevacizumab because of insurance restrictions. After three monthly injections, his NPDR improved, with less NVE and fewer retinal hemorrhages (Figure 13). How often would you recommend bevacizumab for this patient?
Dr. Ali: I’d extend treatment to every 3 to 4 months indefinitely, especially if this patient is compliant. I am not opposed to using anti-VEGF monotherapy in patients with mild PDR, and this case beautifully shows that anti-VEGF monotherapy can be effective in mild PDR.
Dr. Vakharia: My initial challenge was getting this patient to see the benefits of monthly injections, and it’s hard for a pilot to have a follow-up that often. So, I did extend his treatment to bimonthly then quarterly, but as I extended, some NVE and nonperfusion returned. This was likely due to the use of bevacizumab. His 8-month follow-up after six bevacizumab injections revealed that his NVE returned minimally and that retinal edema did not develop. My current goal with this patient is to switch him to a more durable agent for DR, such as aflibercept 2 mg and 8 mg, ranibizumab, or biosimilar ranibizumab. Notably, faricimab is not approved for the primary treatment of diabetic retinopathy without edema.
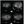 Figure 13. FA imaging in 2017 after three monthly injections of anti-VEGF therapy.
Figure 13. FA imaging in 2017 after three monthly injections of anti-VEGF therapy.
1. Williams AM, Weed JM, Commiskey PW, Kalra G, Waxman EL. Prevalence of diabetic retinopathy and self-reported barriers to eye care among patients with diabetes in the emergency department: the diabetic retinopathy screening in the emergency department (DRS-ED) study. BMC Ophthalmol. 2022;22(1):237.
2. Jansen ME, Krambeer CJ, Kermany DS, et al. Appointment compliance in patients with diabetic macular edema and exudative macular degeneration. Ophthalmic Surg Lasers Imaging Retina. 2018;49(3):186-190.
3. Glassman AR, Wells JA 3rd, Josic K, et al. Five-year outcomes after initial aflibercept, bevacizumab, or ranibizumab treatment for diabetic macular edema (Protocol T Extension Study). Ophthalmology. 2020;127(9):1201-1210.
4. Ehlken C, Helms M, Böhringer D, Agostini HT, Stahl A. Association of treatment adherence with real-life VA outcomes in AMD, DME, and BRVO patients. Clin Ophthalmol. 2017;12:13-20.
5. Brown DM, Boyer DS, Do DV, et al. Intravitreal aflibercept 8 mg in diabetic macular oedema (PHOTON): 48-week results from a randomised, double-masked, non-inferiority, phase 2/3 trial. Lancet. 2024;403(10432):1153-1163.
6. Wykoff CC, Abreu F, Adamis AP, et al. Efficacy, durability, and safety of intravitreal faricimab with extended dosing up to every 16 weeks in patients with diabetic macular oedema (YOSEMITE and RHINE): two randomised, double-masked, phase 3 trials. Lancet. 2022;399(10326):741-755.
7. Ruia S, Tripathy K. Fluorescein Angiography. In: StatPearls [Internet]. StatPearls Publishing; 2024 Jan-. Updated August 25, 2023. Accessed September 23, 2024. https://www.ncbi.nlm.nih.gov/books/NBK576378/
8. Toto L, Romano A, Pavan M, et al. A deep learning approach to hard exudates detection and disorganization of retinal inner layers identification on OCT images. Sci Rep. 2024;14:16652.
9. Baker CW, Glassman AR, Beaulieu WT, et al. Effect of initial management with aflibercept vs laser photocoagulation vs observation on vision loss among patients with diabetic macular edema involving the center of the macula and good visual acuity: a randomized clinical trial. JAMA. 2019;321(19):1880-1894.
10. Regeneron. Eylea HD Package Insert. https://www.regeneron.com/downloads/eyleahd_fpi.pdf. Revised December 2023. Accessed October 9, 2024.
11. Genentech. Vabysmo Package Insert. https://www.gene.com/download/pdf/vabysmo_prescribing.pdf. Revised July 2024. Accessed October 9, 2024.
12. Wells JA, Glassman AR, Ayala AR, et al. Aflibercept, bevacizumab, or ranibizumab for diabetic macular edema: two-year results from a comparative effectiveness randomized clinical trial. Ophthalmology. 2016;123(6):1351-1359.
13. Callari M. Retinal treatments don’t just cost the price on the package. Medscape. Accessed October 9, 2024. https://www.medscape.com/viewarticle/retinal-treatments-dont-just-cost-price-package-2024a1000eqi?form=fpf
14. Patel NA, Al-Khersan H, Yannuzzi NA, Lin J, Smiddy WE. Aflibercept monotherapy versus bevacizumab-first for diabetic macular edema: a cost analysis based on diabetic retinopathy clinical research network Protocol AC results. Ophthalmol Retina. 2023;7(5):413-419.
15. AbbVie Inc. Ozurdex Package Insert. https://www.rxabbvie.com/pdf/ozurdex_pi.pdf. Revised May 2024. Accessed October 10, 2024.
16. Zhang W, Zhao G, Fan W, Zhao T. Panretinal photocoagulation after or prior to intravitreal conbercept injection for diabetic macular edema: a retrospective study. BMC Ophthalmol. 2021;21(1):160.
17. Alsoudi AF, Wai KM, Koo E, Parikh R, Mruthyunjaya P, Rahimy E. Initial therapy of panretinal photocoagulation vs anti-vegf injection for proliferative diabetic retinopathy. JAMA Ophthalmol. Published online August 29, 2024.
18. Writing Committee for the Diabetic Retinopathy Clinical Research Network, Gross JG, Glassman AR, et al. Panretinal photocoagulation vs intravitreous ranibizumab for proliferative diabetic retinopathy: a randomized clinical trial. JAMA. 2015;314(20):2137-2146.
19. Boyer DS, Yoon YH, Belfort R Jr, et al. Three-year, randomized, sham-controlled trial of dexamethasone intravitreal implant in patients with diabetic macular edema. Ophthalmology. 2014;121(10):1904-1914.
20. Alimera Sciences, Inc. Iluvien Package Insert. https://iluvien.com/wp-content/uploads/2024/01/Prescribing-Information.pdf. Revised November 2016. Accessed October 10, 2024.
21. Campochiaro PA, et al. Sustained delivery fluocinolone acetonide vitreous inserts provide benefit for at least 3 years in patients with diabetic macular edema. Ophthalmology. 2012;119(10):2125-2132. doi:10.1016/j.ophtha.2012.04.030
22. Wykoff CC, Yu HJ, Avery RL, Ehlers JP, Tadayoni R, Sadda SR. Retinal non-perfusion in diabetic retinopathy. Eye (Lond). 2022;36(2):249-256.
23. Feldman-Billard S, Larger É, Massin P; Standards for screening and surveillance of ocular complications in people with diabetes SFD study group. Early worsening of diabetic retinopathy after rapid improvement of blood glucose control in patients with diabetes. Diabetes Metab. 2018;44(1):4-14.
24. Early Treatment Diabetic Retinopathy Study Research Group. Fundus photographic risk factors for progression of diabetic retinopathy. ETDRS report number 12. Early Treatment Diabetic Retinopathy Study Research Group. Ophthalmology. 1991;98(5 Suppl):823-833.
25. Yonekawa Y, Modi YS, Kim LA, Skondra D, Kim JE, Wykoff CC. American Society of Retina Specialists Clinical Practice Guidelines on the Management of Nonproliferative and Proliferative Diabetic Retinopathy without Diabetic Macular Edema. J Vitreoretin Dis. 2020;4(2):125-135.
26. FAA field of vision requirements. Left Seat. Accessed September 24, 2024. https://www.leftseat.com/field-of-vision-faa-medical-certification-requirements-2/
Advancing Treatment Strategies for Better Outcomes in nAMD
Neovascular age-related macular degeneration (nAMD) remains a leading cause of vision loss in older adults despite use of anti-VEGF therapies.1,2 Early detection and timely intervention are critical; however, patients often face challenges such as delayed diagnosis, progressive vision loss, and limited access to optimal care.1 First-generation anti-VEGF agents, including off-label bevacizumab and aflibercept, may be effective but can present challenges in maintaining disease control long-term and requiring frequent follow-up.3 These challenges have prompted a shift toward second-generation therapies, ie, aflibercept 8 mg and faricimab, that offer comparable efficacy but with enhanced durability and flexible dosing.4,5 In a recent closed panel discussion, retina specialists with varying clinical experience shared the following seven cases that include real-world management approaches for patients with nAMD.
— Priya S. Vakharia, MD
CASE 1: A PATIENT SWITCHED FROM AFLIBERCEPT 2 MG TO FARICIMAB AFTER FAILING EXTENSION
Jayanth Sridhar, MD: Our first AMD case is a 76-year-old female with a history of dry AMD OU who was referred for wavy vision in her left eye and had been on AREDS supplementation for 7 years. An OCT showed drusen in her right eye, and a large pigment epithelial detachment (PED) in their left eye; each eye had subretinal and intraretinal fluid (SRF and IRF). Her VA was 20/150 OS (Figure 1A). One month after an aflibercept 2 mg injection in the left eye, her vision improved significantly to 20/40-2, and her PED resolved (Figure 1B).
Unfortunately, after five monthly aflibercept injections, we attempted to extend to 6 weeks, but SRF recurred (Figure 2A). We gave the patient a seventh dose of aflibercept 2 mg, and 4 weeks later her IRF increased dramatically (Figure 2B). Given the good initial response to aflibercept 2 mg, the likelihood of vitreomacular traction is low. Dr. Warren, what would you do when a patient responds well initially but struggles with extension?
Alexis Warren, MD: It depends on the patient, but I’d typically shorten the interval again for a few injections and try again later to extend. If the patient can’t visit for follow-ups frequently, I may consider switching to a drug with better durability. It’s important to have a conversation with the patient.
Matthew Starr, MD: I agree that this treatment decision is patient dependent. I would determine the patient's goals and explain my goals of improving vision and extending treatment intervals as much as possible. Aflibercept 2 mg injections are perhaps the gold standard of our current treatment algorithms, so I wouldn’t switch this patient unless they are eager to try something different.
 Figure 1. OCT imaging at baseline (A) and one month after aflibercept 2 mg (B).
Figure 1. OCT imaging at baseline (A) and one month after aflibercept 2 mg (B).
 Figure 2. OCT imaging 6 weeks after five monthly aflibercept 2 mg injections (A) and 4 weeks after seventh aflibercept 2 mg injection (B).
Figure 2. OCT imaging 6 weeks after five monthly aflibercept 2 mg injections (A) and 4 weeks after seventh aflibercept 2 mg injection (B).
Allen C. Ho, MD, FACS, FASRS: It is uncommon to observe a sudden reversal in treatment response like in this case; treatment responses in nAMD are usually consistent. I would confirm the diagnosis and then consider aflibercept 8mg or faricimab.
Jordan Deaner, MD: I’d also question the diagnosis and perform further testing, like fluorescein angiography (FA) or OCTA, to confirm neovascular disease. If nAMD is confirmed, then I’d probably switch to a second-generation therapy, specifically faricimab in this case, the only dual-pathway agent.6
Nita Valikodath, MD, MS: I agree with further workup to confirm the diagnosis. I’m uncomfortable tolerating this degree of SRF after five aflibercept 2 mg injections and if I’m sure the drug entered the eye, I would consider switching to faricimab.
Dr. Sridhar: With the FDA approval of two second-generation therapies, faricimab and aflibercept 8 mg, how do you decide which drug to switch to?
Samuel Minaker, MD: Because of this patient’s dramatic response initially, I may have tried aflibercept 8 mg to extend, which may increase durability and enhance the drying effect.7 However, after the patient’s dramatic regression, I’d switch to faricimab.
Dr. Sridhar: We did switch this patient to faricimab, and after one dose her VA improved to 20/30, and her retinal fluid decreased dramatically (Figure 3). Would anyone extend now?
Barton Lynn Blackorby, MD: I usually change only one aspect of treatment at a time, meaning either the drug or the interval. For example, if I switch drugs and see less fluid and the same visual acuity, then I will extend the interval with the same drug for the next visit.
 Figure 3. OCT imaging 4 weeks after switch to faricimab.
Figure 3. OCT imaging 4 weeks after switch to faricimab.
Dr. Sridhar: Notably, after the loading doses in the major clinical trials TENAYA and LUCERNE, which evaluated the efficacy and safety of faricimab in nAMD, the extensions were aggressive using a prn approach for a treatment interval of 8, 12, and 16 weeks.5 These extensions were essentially 1-month intervals, whereas most of us in real-world practice extend by 1 to 2 weeks. Dr. Park, when do you start extending on a new drug and how aggressive are your extensions?
Jong Park, MD: If this patient’s retina had been dry after the three loading doses, then I’d extend by 1 or 2 weeks each time, but I’d be very cautious given the earlier recurrence of fluid.
Dr. Starr: I also think it is too soon to extend. I’d probably reload them.
Dr. Sridhar: I have observed that retina specialists do not often reload patients in real-world settings, whereas patients in clinical trials are often reloaded. To continue, our plan for this patient was monthly faricimab injections, given our cautiousness surrounding the fluid recurrence previously. If this patient had been unhappy, then we’d have to reconsider the drug or dosing interval.
Dr. Vakharia: I want to bridge a point here about retinal fluid tolerance. Historically, we aimed for a completely dry retina, but trials are now tolerating more fluid in patients.5 Are we starting to tolerate more fluid?
Dr. Ho: I don’t know whether we are tolerating fluid more as a community, but clinical trials are pushing the threshold for fluid tolerance to validate claims for durability. Importantly, the location of the retinal fluid determines my tolerance. SRF is less damaging than IRF8,9; so, I’m more tolerant of it. In clinical practice, I will typically extend more cautiously by 1-to-2-week intervals rather than by the monthly intervals that we see in some clinical trials.
Dr. Sridhar: In the past, we were strict about eliminating all fluid. Now, we are in an era where the focus of trials is on improving anti-VEGF durability by meeting certain endpoints. We need to carefully evaluate the data of trials by considering the patient’s individual response before extending treatment intervals. Notably, a 2022 real-world study examining the effect of retinal fluid tolerance on the visual outcomes of patients with nAMD showed that tolerating small amounts of fluid of 50 mm or less can give comparable VA results without significant risk.10
Dr. Vakharia: I agree that trial design and retreatment criteria often influence patient results and outcomes in the real world. We need to manage patient expectations for treatment durability.
CASE 2: A 70-YEAR-OLD MALE WITH nAMD AND PERSISTENT FLUID AFTER MONTHLY RANIBIZUMAB
Dr. Ho: This AMD case involves a 70-year-old male with a history of nAMD, presenting with a VA of 20/80 OS. His OCT in the left eye showed SRF, a PED, subretinal hyperreflective material (SHRM), and minimal IRF (Figure 4A). After three monthly ranibizumab injections, his VA improved to 20/60, and the IRF and SHRM reduced some but persisted (Figure 4B). Dr. Starr, what would you do next?
Dr. Starr: I am not a proponent of switching medications early. I think patients who receive three monthly injections and have a response, even if it’s suboptimal initially, can benefit from an additional 1 to 3 months of injections before switching medications.
 Figure 4. OCT in the left eye showed SRF, a PED, SHRM, and minimal IRF (A). After three monthly ranibizumab injections, the IRF and SHRM reduced some but persisted (B).
Figure 4. OCT in the left eye showed SRF, a PED, SHRM, and minimal IRF (A). After three monthly ranibizumab injections, the IRF and SHRM reduced some but persisted (B).
Dr. Park: It’s a tough decision. If you switch agents and the patient improves, you feel great; if the patient gets worse, you regret the switch. I’d also recommend a few more injections and prepare the patient for a potential switch. I’d recheck the patient again 1 month after the fourth injection.
Dr. Valikodath: I agree. Here, we’re seeing improvement in vision and on OCT. I’d also discuss with the patient whether they are noticing subjective improvement. I also like to discuss alternative treatment options early in the process so that they are prepared when the time comes to switch agents.
Dr. Ho: Good point about patient communication. Most of us encounter insurance barriers, so switching medications requires planning ahead for the next visit. In this case, the patient was switched to aflibercept 2 mg for three injections, which slightly improved his VA to 20/50, although some fluid remained.
Dr. Warren: I wouldn’t have switched initially, but I like the anatomical and visual results. I’d now continue with aflibercept 2 mg and manage patient expectations regarding future injections. They need to understand that improvement may be limited and that long-term, frequent injections may be necessary.
Dr. Ho: Good point. I always tell patients, “We’ll do our best and review scans together to track progress. I don’t know yet if your treatment will be lifelong. We’ll do whatever it takes to get you as good as possible and choose the treatment that’s compatible with your lifestyle.”
Most patients want good vision, and a key determinant in visual outcomes is the presenting acuity when the patient first presents with the disease.11 A 2020 retrospective study of IRIS registry patients with nAMD in one or both eyes evaluated long-term visual outcomes in the treated eye after two or more anti-VEGF injections.11 This study found that patients with 20/40 VA or better at baseline continued with a VA of 20/40 or better for 2 years after starting treatment.11 Therefore, the earlier we detect nAMD, the better the prognosis. Unfortunately, only 34% of patients in the IRIS registry diagnosed with nAMD had 20/40 VA or better at presentation.11
Use of an in-home monitoring device may benefit patients and preserve their vision. In a real-world study evaluating patients with intermediate AMD using an in-home monitoring device, about 80% maintained a VA of 20/40 or better when the device detected conversion to wet AMD.12 In addition, we can emphasize to patients to monitor their vision with Amsler grids, use the cross-cover technique when checking vision, and schedule an appointment for any vision changes. Clinically, we can scan both eyes at every visit in patients with AMD who are receiving monocular injections to help catch worsening disease early in the fellow eye.
CASE 3: TREATMENT EXTENSION IN A PATIENT WITH PERSISTENT SRF
Dr. Vakharia: This case involves a 66-year-old male previously diagnosed with nAMD in the right eye who presented with a VA of 20/50 and SRF. This clinical presentation is common, similar to patients in faricimab’s clinical trials (TENAYA and LUCERNE), in which the average incoming VA was about 20/63.5 After four loading doses of aflibercept 2 mg dosed every 4 weeks, this patient’s VA improved to 20/25, although some SRHM remained (Figure 5A). Who here would extend this patient to 6 weeks?
Dr. Sridhar: I wouldn’t extend this patient to 6 weeks because of their SRHM, which indicates active disease and is associated with recurrence and poor outcomes.13 I treat all SHRM like blood, meaning I inject monthly until clinically resolved.
Dr. Vakharia: That’s a great point. I, however, extended this patient to 6 weeks, but the patient had recurrent fluid, and their VA declined to 20/40. Most of us in the real world would shorten this patient’s interval due to worsening fluid and worsening visual acuity. In fact, even in the phase 3 clinical trial PULSAR, which studied the efficacy and safety of aflibercept 8 mg in nAMD, interval shortening occurred in patients who had worsening central subfield thickness (CST) and vision loss.4 I shortened the interval for this patient back to 4 weeks but also switched this patient to faricimab and administered three doses of faricimab every 4 weeks, then extended to 6 weeks for comparison (Figure 5B).
 Figure 5. OCT imaging 6 weeks after four loading doses of aflibercept 2 mg (A) and 6 weeks after three monthly doses of faricimab (B).
Figure 5. OCT imaging 6 weeks after four loading doses of aflibercept 2 mg (A) and 6 weeks after three monthly doses of faricimab (B).
Although some fluid remained at the 6-week follow-up on faricimab, I decided to extend the patient to 8 weeks. Their OCT looked good at the 8-week follow-up with only a sliver of SRF. Sometimes, I find that with time, patients start to get better fluid control after multiple doses of their anti-VEGF agent, and perhaps even further extension can be attempted in the future. Therefore, even if a patient has failed an extension one time, I sometimes will reattempt this extension later.
Dr. Warren: Sometimes the more exposure real-world patients have to the medication, the more we can extend. We’re not sure why this happens, and this case shows that it can work out well.
Dr. Vakharia: After a while on 8-week dosing, I then extended him to 10 weeks and he looked stable with good vision and good fluid control, although he still had a small amount of SRF. We know that we can tolerate a very small amount of SRF in wet AMD, but the question is how much? Dr. Deaner, would you stay at 10 weeks, extend to 12 weeks, or switch agents?
Dr. Deaner: With the patient having great vision and minimal SRF, I’d tolerate it as long as they remain stable and asymptomatic. I’m cautious with extensions; I’d slowly extend this patient to 11 weeks.
Dr. Sridhar: The major trials TENAYA and LUCERNE suggest that 1-month extensions are safe in patients receiving faricimab who meet the criteria.5 However, in practice, we’re more conservative with shorter extensions.
Dr. Ho: I don’t agree with every trial’s retreatment criteria, and I only participate in trials that allow the investigator to dictate what’s best for the patient. I also tend to extend my patients by 1 to 2 weeks, not a full month. Again, I’ve become more tolerant of SRF over time, but I usually avoid extending when there’s IRF, which is more likely to impact vision.
CASE 4: A CASE OF QUICK EXTENSION WITH AFLIBERCEPT 8 MG IN A PATIENT WITH STABLE OUTCOMES
Dr. Vakharia: An 80-year-old female presented with early nAMD in her right eye. She received three doses of aflibercept 8 mg 1 month apart. Her OCT at 28 days after the third dose showed absence of fluid, and her VA improved to 20/20 (Figure 6). I’m forced to extend this patient to 7 or 8 weeks for her fourth dose of aflibercept 8 mg according to its label.7 How do we feel about this extension?
Dr. Ho: I’m not comfortable with this extension, so I administer aflibercept 8 mg less frequently. However, I’ve administered aflibercept 8 mg for patients with recalcitrant fluid and got some response. My go-to drug remains aflibercept 2 mg, which works well in most cases needing anti-VEGF therapy. I look forward to studies allowing more frequent dosing of aflibercept 8 mg, which hopefully will change the labeling.
Dr. Park: I’m also uncomfortable with the extension criteria with aflibercept 8 mg because I haven’t used this approach with any other medication. During my training and fellowship, the attending physicians didn’t jump from 4-week to 8-week intervals, so this extension feels foreign to me.
 Figure 6. OCT imaging 28 days after second dose of aflibercept 8 mg.
Figure 6. OCT imaging 28 days after second dose of aflibercept 8 mg.
Dr. Blackorby: I agree. It’s hard to jump from a dosing interval of 4 to 8 weeks and, importantly, patients often resist big changes in their intervals because they’re used to small incremental increases. However, in this case with complete resolution of SRF, I may take the risk and extend this patient to 8 weeks.
Dr. Vakharia: I extended this patient to about 7 or 8 weeks, and at 52 days postinjection, some fluid returned superior to the fovea, and her VA remained 20/20. If participating in the clinical trial, this patient would have been extended further according to the trials’ extension criteria,4 but what should our approach be in the real world?
Dr. Minaker: I’ve had similar cases with aflibercept 8 mg. Typically, I tend to stay cautious, keeping the same interval when there’s fluid. Nevertheless, some patients push for longer intervals, making me tolerate more fluid than I like, and their results with aflibercept 8 mg have surprised me in a good way.
Dr. Deaner: I think that when a patient has decreased fluid and good vision, it’s worth trying to extend. Although I’m cautious and typically consider a single-week extension only, extending by 2 weeks with newer agents seems less risky. It’s important to have a conversation with the patient.
Dr. Vakharia: This response from all of you here highlights the disconnect between treating patients with clinical trial protocols versus real-world practice. For this patient, I gave her another dose after 57 days postinjection and extended her to 10 weeks.
Dr. Starr: Because this patient has been stable, I think a 10-week extension is reasonable. This case represents ideal outcomes from treatment with aflibercept 8 mg, which allows for quick extension.7
CASE 5: SUBMACULAR HEMORRHAGE—SURGERY VERSUS ANTI-VEGF THERAPY
Dr. Ho: This patient is an 82-year-old female with a central disciform scar in her right eye and a history of hemorrhages in both eyes. She presented with early AMD, but her OCT showed a submacular hemorrhage in her left eye with a VA of 20/200 (Figure 7). I usually treat central thick submacular hemorrhages with surgery with submacular tissue plasminogen activator (TPA), and I use an intraocular air bubble to displace the blood. However, in this case, the blood wasn’t thick in the central macula, so I didn’t opt for surgery.
Dr. Blackorby: I agree that surgery isn’t necessary with a centrally clear macula. As opposed to administering a first-generation agent with submacular hemorrhages, I go straight to faricimab because it has a quick drying effect and treats multiple disease pathways. I want the broadest spectrum of action to shut the CNVM down as quickly as possible.5
Dr. Starr: The monocular status of this patient makes this case challenging. I would consider subretinal TPA surgery. For me, the decision to elect for surgery depends on the patient's functional status. If the patient is aiming for a “home run” or significant improvement, surgery may be a good option. Otherwise, starting right away with intravitreal injections is imperative.
Dr. Warren: I agree. Here, I’d discuss vision expectations with the patient, especially given the history in the right eye. I’d also talk extensively about how aggressive we want to be and how this decision may affect potential costs if we switch to an alternative therapy later.
Dr. Valikodath: Yes, I’d switch to aflibercept 8 mg or faricimab as soon as possible. Setting realistic expectations early on visual recovery is crucial. I like to show patients their OCT images and explain which retinal findings may remain and limit their vision after treatment.
Dr. Ho: After this patient received five anti-VEGF injections every 4 weeks, their retinal blood cleared, but their VA remained 20/200, indicating a more central retinal pigment epithelium (RPE) tear (Figure 8). In addition, this patient was on aspirin. How do you manage antiplatelet and anticoagulant use in a patient with a retinal hemorrhage?
 Figure 7. Fundus photo (A) and OCT (B) showing submacular hemorrhage.
Figure 7. Fundus photo (A) and OCT (B) showing submacular hemorrhage.
 Figure 8. OCT image (A) and fundus photo (B) at 6 month follow-up.
Figure 8. OCT image (A) and fundus photo (B) at 6 month follow-up.
Dr. Vakharia: Unless it’s a case of a suprachoroidal hemorrhage, I don’t stop anticoagulation therapy for macular hemorrhages. The only instances that I will stop anticoagulation therapy for macular hemorrhages are if the anticoagulation therapy is prophylactic or no longer necessary. I do worry about the risk of strokes when anticoagulants are discontinued.14
Dr. Deaner: If patients are on prophylactic aspirin without a history of cardiovascular incident or stroke, then I have them stop their aspirin. However, if they’re on a therapeutic dose of an antiplatelet or anticoagulant medication for atrial fibrillation or they have stents or a history of cardiovascular incidents, then I consult with their cardiologist and discuss the patient’s ocular disease and need for retinal treatment. I don’t pressure the cardiologist to stop the patient’s anticoagulant therapy, unless the patient has a suprachoroidal hemorrhage.
Dr. Ho: Retrospective studies suggest that anticoagulant use does not increase the risk of bleeding in AMD but can be associated with more severe bleeds if it is to occur.15,16 My approach with patients on anticoagulant medication is similar to Dr. Deaner’s.
Dr. Sridhar: For patients on the fence about retinal surgery, I often inject them with anti-VEGF therapy first and schedule their surgery within 10 to 14 days. Sometimes, the injection improves the retinal anatomy on OCT and how the patient feels psychologically, and the patient then decides against surgery. A study by Chang et al showed that managing submacular hemorrhages with surgery alone versus adding postoperative anti-VEGF therapy significantly improved vision for the first 6 months, but vision declined over time.17 Furthermore, there are no studies showing that displacement surgery for nAMD results in better outcomes than treating with anti-VEGF therapy. Taken together, this evidence has raised my threshold for recommending surgery.
Dr. Ho: Good points. I rarely perform subretinal TPA surgery, but when aiming for a “home run” result, it can be worth the risk, in my opinion. Because large bleeds are often associated with an RPE tear, the location of the tear and the extent of subretinal fibrosis influence vision after blood resorbs.
CASE 6: A PATIENT WITH A SIGNIFICANT PED REQUIRING TREATMENT IN BOTH EYES
Dr. Sridhar: Our sixth case is a 72-year-old female with a history of dry AMD, observed by an optometrist every 6 months. She had a history of smoking from 20 years prior and supplemented with AREDS2 for 10 years. She was referred for possible conversion to nAMD in the right eye. However, she waited 2 months for her scheduled appointment for insurance eligibility. She presented with a VA of 20/100 OD, and her fundus photos showed some hemorrhaging and central drusen within the posterior pole. Her left eye had a VA of 20/50 and several large drusen. Her OCT revealed a large PED and SHRM in her right eye and drusen only in her left eye (Figure 9). With this presentation, I’m concerned about a potential RPE rip due to the steep M-shaped PED on the temporal side of her macula. Does anyone modify their drug choice because of this risk?
Dr. Minaker: I’d be cautious about flattening a large PED with a second-generation agent (ie, faricimab or aflibercept 8 mg). I’d start with traditional step therapy with a first-generation agent (ie, ranibizumab, aflibercept 2 mg, or off-label bevacizumab) to shrink the PED first, particularly when there’s also a small versus large hemorrhage.
Dr. Warren: In my 1 year of clinical experience, I haven’t changed my drug choice with this presentation, but it’s worth considering. Luckily, I haven’t had a patient develop an RPE tear.
Dr. Vakharia: I’ve had patients in whom their RPE ripped. Although it’s not evidence based, I like to start with bevacizumab to reduce the PED before switching to a stronger agent as well.
Dr. Sridhar: Our approaches are retina “voodoo,” as we like to call it. Without solid evidence, we each have an individual approach. I think that sometimes management of retinal disease is an attempt to present an illusion of control. Some doctors are conservative in their agent choice, whereas others choose the strongest drug immediately. The worst approach in this case is to withhold anti-VEGF therapy.
Dr. Vakharia: Patients want to feel in control. If a patient requests a specific drug because of a bad outcome with another drug, then I consider their preference to give them a sense of control.
Dr. Sridhar: We recommended monthly injections; however, the patient had to select a different retina specialist due to travel restrictions. She returned to us 2 years later because she moved closer. Over 2 years, she had received a total of 10 injections in her right eye, starting with two injections of bevacizumab before switching to faricimab because of a worsening hemorrhage (Figure 10). She’s up to every-4-month intervals with faricimab. Her VA stabilized at 20/40 OD and 20/50 OS. Her OCT showed that a small RPE rip may have occurred in her right eye and that IRF has now developed in her left eye. Does the first eye’s response influence your choice of agent for the fellow eye?
 Figure 9. Baseline OCT images.
Figure 9. Baseline OCT images.
 Figure 10. OCT images 2 years s/p 10 injections (two off-label bevacizumab; eight faricimab) OD and treatment-naïve OS
Figure 10. OCT images 2 years s/p 10 injections (two off-label bevacizumab; eight faricimab) OD and treatment-naïve OS
Dr. Valikodath: I still follow step therapy because of patient preference due to insurance constraints. I do submit appeals but the timing may not work out if it’s an acute situation. I have a conversation with the patient because they are often nervous about using a drug that didn’t work in the first eye. It’s still ideal to treat promptly with that initial agent than delay care. If the first eye responded well with a certain agent, then I’ll switch sooner to this agent for the fellow eye.
Dr. Sridhar: Dr. Park, how much does the patient’s input influence your choice for the fellow eye?
Dr. Park: Great question, I think the patient ultimately needs to trust your decision-making. If I was constrained by insurance, I’d explain that the situation in the fellow eye is different and that we may need to try bevacizumab again. Without insurance constraints, I’d start with faricimab to gain this patient’s trust and willingness to follow-up.
Dr. Sridhar: Dr. Blackorby, do you try to align the different treatment intervals for each eye?
Dr. Blackorby: It depends. If the patient is local, I’ll keep the different intervals and treat each eye specific to its needs. If they’ve traveled far or transportation is difficult, I attempt to align the treatment intervals. I also will perform bilateral injections to limit the number of appointments.
Dr. Deaner: I try to match treatment intervals or at least find a common divisor. The goal is to reduce the burden on the patient while maintaining their vision. Sometimes I may shorten the interval in one eye and essentially “overtreat” briefly to allow the patient to “live their life” by avoiding frequent visits.
Dr. Park: At my satellite clinics, I err on the side of caution, seeing patients and injecting them sooner rather than later. It’s not ideal, but I’d rather see them more frequently than risk waiting too long.
Dr. Vakharia: Great point, retina specialists can increase patient access to care by utilizing satellite clinics.
CASE 7: A PATIENT WITH nAMD AND DEVELOPING GA
Dr. Vakharia: Our last case is an 85-year-old, pseudophakic female with nAMD who received multiple aflibercept 2 mg injections and presented for follow-up. Her most recent injection was 8 months prior. An OCT of the left eye showed a dry retina and a VA of 20/50 (Figure 11A). We decided to monitor her (Figure 11B) and 2 years later her VA had progressively worsened to counting fingers at 1 ft, despite no neovascular activity (Figure 11C). At this point, her OCT showed choroidal hypertransmission suggestive of geographic atrophy (GA). This case highlights that patients with nAMD, even actively treated patients, can lose vision from GA. How do you handle conversations with patients who expect to maintain their vision because they were told their condition was treatable but who experience further vision loss?
Dr. Warren: These conversations are often long and dissatisfying to the patient. I explain that some aspects of AMD, like fluid, are treatable but that some cells degenerate, which treatment can’t stop. I try to add a positive note by mentioning ongoing research in AMD but explain that we don’t have all the answers yet.
Dr. Vakharia: Would anyone start anticomplement therapy, including pegcetacoplan and avacincaptad pegol, to treat this patient’s GA?18,19
Dr. Sridhar: I’m hesitant to administer complement inhibitors (CIs) in patients with a history of nAMD because of the conversion risk, especially in the better eye, and its potential to increase the rate of vision loss.18,19 I know some clinicians alternate between anti-VEGF and CI therapy, but we don’t have evidence supporting this approach.
Dr. Blackorby: I do treat some patients with both CI and anti-VEGF therapies. I closely watch patients treated with CIs because of the higher risk of choroidal neovascular membrane.18,19
Dr. Sridhar: Also, I wanted to add an important point about counseling patients. We have all experienced patients who insist on frequent anti-VEGF injections despite not needing them clinically or anatomically, when we advise against them because of unnecessary risk and the debatable potential to worsen atrophy.20-22 When I explain the potential for a worsening prognosis, patients are usually willing to accept my recommendation of less aggressive treatment.
Dr. Ho: Lastly, we’ve made progress in managing AMD during my career, but I think we still need to detect disease earlier to improve long-term patient outcomes. I have hope that potential treatments in development, such as gene therapy and photobiomodulation, will offer improved mechanisms of action to prevent or treat atrophy and preserve vision. It’s also crucial, in my opinion, to shift our focus in research from 6-month or 1-year visual acuity endpoints to day-to-day vision (area under the VA curve), which is the focus of our patients.
 Figure 11. Sequential OCT images and management protocol.
Figure 11. Sequential OCT images and management protocol.
1. Wykoff CC, Garmo V, Tabano D, et al. Impact of anti-VEGF treatment and patient characteristics on vision outcomes in neovascular age-related macular degeneration: up to 6-year analysis of the AAO IRIS® Registry. Ophthalmol Sci. 2023;4(2):100421.
2. Singer M, Singh RP, Gibson A, et al. Association of early anatomic response with visual function in neovascular age-related macular degeneration. Ophthalmology. 2021;128(11):1657-1660.
3. Kaiser SM, Arepalli S, Ehlers JP. Current and future anti-VEGF agents for neovascular age-related macular degeneration. J Exp Pharmacol. 2021;13:905-912.
4. Lanzetta P, Korobelnik JF, Heier JS, et al. Intravitreal aflibercept 8 mg in neovascular age-related macular degeneration (PULSAR): 48-week results from a randomised, double-masked, non-inferiority, phase 3 trial. Lancet. 2024;403(10432):1141-1152.
5. Heier JS, Khanani AM, Quezada Ruiz C, et al. Efficacy, durability, and safety of intravitreal faricimab up to every 16 weeks for neovascular age-related macular degeneration (TENAYA and LUCERNE): two randomised, double-masked, phase 3, non-inferiority trials. Lancet. 2022;399(10326):729-740.
6. Genentech. Vabysmo Package Insert. https://www.gene.com/download/pdf/vabysmo_prescribing.pdf. Revised July 2024. Accessed October 9, 2024.
7. Regeneron. Eylea HD Package Insert. https://www.regeneron.com/downloads/eyleahd_fpi.pdf. Revised December 2023. Accessed October 9, 2024.
8. Chaudhary V, Matonti F, Zarranz-Ventura J, Stewart MW. impact of fluid compartments on functional outcomes for patients with neovascular age-related macular degeneration: a systematic literature review. Retina. 2022;42(4):589-606.
9. Riedl S, Vogl WD, Waldstein SM, Schmidt-Erfurth U, Bogunović H. impact of intra- and subretinal fluid on vision based on volume quantification in the HARBOR trial. Ophthalmol Retina. 2022;6(4):291-297.
10. Jeng YT, Lai TT, Lin CW, et al. The impact of retinal fluid tolerance on the outcomes of neovascular age-related macular degeneration treated using aflibercept: A real-world study. PLoS One. 2022;17(7):e0271999.
11. Ho AC, Kleinman DM, Lum FC, et al. Baseline visual acuity at wet AMD diagnosis predicts long-term vision outcomes: an analysis of the IRIS Registry. Ophthalmic Surg Lasers Imaging Retina. 2020;51(11):633-639.
12. Ho AC, Heier JS, Holekamp NM, et al. Real-world performance of a self-operated home monitoring system for early detection of neovascular age-related macular degeneration. J Clin Med. 2021;10(7):1355.
13. Feo A, Stradiotto E, Sacconi R, Menean M, Querques G, Romano MR. Subretinal hyperreflective material in retinal and chorioretinal disorders: A comprehensive review. Surv Ophthalmol. 2024;69(3):362-377.
14. García Rodríguez LA, Cea Soriano L, Munk Hald S, et al. Discontinuation of oral anticoagulation in atrial fibrillation and risk of ischaemic stroke. Heart. 2020;107(7):542-548.
15. Ying GS, Maguire MG, Daniel E, et al. Association between antiplatelet or anticoagulant drugs and retinal or subretinal hemorrhage in the comparison of age-related macular degeneration treatments trials. Ophthalmology. 2016;123(2):352-360.
16. Weber C, Bertelsmann M, Kiy Z, Stasik I, Holz FG, Liegl R. Antiplatelet and anticoagulant therapy in patients with submacular hemorrhage caused by neovascular age-related macular degeneration. Graefes Arch Clin Exp Ophthalmol. 2023;261(5):1413-1421.
17. Chang W, Garg SJ, Maturi R, et al. Management of thick submacular hemorrhage with subretinal tissue plasminogen activator and pneumatic displacement for age-related macular degeneration. Am J Ophthalmol. 2014;157(6):1250-1257.
18. Apellis. Syfovre Package Insert. https://pi.apellis.com/files/PI_SYFOVRE.pdf. Revised November 2023. Accessed October 10, 2024.
19. Astellas Pharma US, Inc. Izervay Package Insert. https://www.astellas.com/us/system/files/izervay_pi.pdf. Revised February 2024. Accessed October 10, 2024.
20. Abdelfattah NS, Zhang H, Boyer DS, Sadda SR. Progression of macular atrophy in patients with neovascular age-related macular degeneration undergoing antivascular endothelial growth factor therapy. Retina. 2016;36(10):1843-1850.
21. Lois N, McBain V, Abdelkader E, Scott NW, Kumari R. Retinal pigment epithelial atrophy in patients with exudative age-related macular degeneration undergoing anti-vascular endothelial growth factor therapy. Retina. 2013;33(1):13-22.
22. Young M, Chui L, Fallah N, et al. Exacerbation of choroidal and retinal pigment epithelial atrophy after anti-vascular endothelial growth factor treatment in neovascular age-related macular degeneration. Retina. 2014;34(7):1308-1315.


 Figure 1. Baseline OCT.
Figure 1. Baseline OCT. Figure 2. FA imaging.
Figure 2. FA imaging. Figure 3. Baseline OCT.
Figure 3. Baseline OCT. Figure 4. OCT imaging after third dose of aflibercept 8 mg.
Figure 4. OCT imaging after third dose of aflibercept 8 mg. Figure 5. OCT imaging from first through fourth anti-VEGF injection.
Figure 5. OCT imaging from first through fourth anti-VEGF injection. Figure 6. Baseline OCT imaging.
Figure 6. Baseline OCT imaging. Figure 7. OCT imaging after five intravitreal injections of anti-VEGF therapy.
Figure 7. OCT imaging after five intravitreal injections of anti-VEGF therapy. Figure 8. OCT imaging 5 months after second dexamethasone intravitreal implant.
Figure 8. OCT imaging 5 months after second dexamethasone intravitreal implant. Figure 9. Baseline FA imaging.
Figure 9. Baseline FA imaging. Figure 10. Baseline OCT (A), final OCT 5 years later (B).
Figure 10. Baseline OCT (A), final OCT 5 years later (B). Figure 11. OCT imaging in 2017 at time of PDR diagnosis.
Figure 11. OCT imaging in 2017 at time of PDR diagnosis. Figure 12. Baseline FA imaging in 2017 before treatment.
Figure 12. Baseline FA imaging in 2017 before treatment. Figure 13. FA imaging in 2017 after three monthly injections of anti-VEGF therapy.
Figure 13. FA imaging in 2017 after three monthly injections of anti-VEGF therapy. Figure 1. OCT imaging at baseline (A) and one month after aflibercept 2 mg (B).
Figure 1. OCT imaging at baseline (A) and one month after aflibercept 2 mg (B). Figure 2. OCT imaging 6 weeks after five monthly aflibercept 2 mg injections (A) and 4 weeks after seventh aflibercept 2 mg injection (B).
Figure 2. OCT imaging 6 weeks after five monthly aflibercept 2 mg injections (A) and 4 weeks after seventh aflibercept 2 mg injection (B). Figure 3. OCT imaging 4 weeks after switch to faricimab.
Figure 3. OCT imaging 4 weeks after switch to faricimab. Figure 4. OCT in the left eye showed SRF, a PED, SHRM, and minimal IRF (A). After three monthly ranibizumab injections, the IRF and SHRM reduced some but persisted (B).
Figure 4. OCT in the left eye showed SRF, a PED, SHRM, and minimal IRF (A). After three monthly ranibizumab injections, the IRF and SHRM reduced some but persisted (B).  Figure 5. OCT imaging 6 weeks after four loading doses of aflibercept 2 mg (A) and 6 weeks after three monthly doses of faricimab (B).
Figure 5. OCT imaging 6 weeks after four loading doses of aflibercept 2 mg (A) and 6 weeks after three monthly doses of faricimab (B). Figure 6. OCT imaging 28 days after second dose of aflibercept 8 mg.
Figure 6. OCT imaging 28 days after second dose of aflibercept 8 mg. Figure 7. Fundus photo (A) and OCT (B) showing submacular hemorrhage.
Figure 7. Fundus photo (A) and OCT (B) showing submacular hemorrhage. Figure 8. OCT image (A) and fundus photo (B) at 6 month follow-up.
Figure 8. OCT image (A) and fundus photo (B) at 6 month follow-up. Figure 9. Baseline OCT images.
Figure 9. Baseline OCT images. Figure 10. OCT images 2 years s/p 10 injections (two off-label bevacizumab; eight faricimab) OD and treatment-naïve OS
Figure 10. OCT images 2 years s/p 10 injections (two off-label bevacizumab; eight faricimab) OD and treatment-naïve OS Figure 11. Sequential OCT images and management protocol.
Figure 11. Sequential OCT images and management protocol.