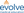Primary open-angle glaucoma (POAG) is a chronic, progressive eye disease in which optic nerve damage causes visual field loss and eventual irreversible blindness if untreated. POAG is a significant public health problem, affecting approximately 76 million people globally.1 It is the second leading cause of blindness worldwide, but the leading cause of blindness in African Americans. Reducing intraocular pressure (IOP) is the most important treatable risk factor in glaucoma management. There are a variety of strategies to control IOP, depending upon the severity of the disease and needs of the patient, including medical therapy, selective laser trabeculoplasty (SLT), minimally invasive glaucoma surgery (MIGS), and invasive procedures like trabeculectomy.1 With so many options in our armamentarium, clinicians must create personalized treatment plans based on patient preferences and factors unique to each case. The following educational supplement brings together thought leaders in glaucoma to discuss and debate challenging real-world cases for which there is no single right answer.
— Douglas J. Rhee, MD, Program Chair
ROUND 1 | CASE 1: PRE-PERIMETRIC GLAUCOMA WITHOUT VISUAL FIELD LOSS
Dr. Rhee: Can there be glaucoma without visual field changes?
Our first case is a 67-year-old self-identified male of European ancestry, who presents for a glaucoma evaluation due to suspicious optic nerves. VA is 20/25 OU, and his IOP is 18 mm Hg OD and 17 mm Hg OS. His central corneal thickness (CCT) is average: 540 µm OD and 550 µm OS. The slit lamp exam is only positive for trace nuclear sclerosis (NS). Gonioscopy is open. His visual fields are shown in Figure 1. Dr. Radcliffe, what are your observations?
Nathan M. Radcliffe, MD: The first thing that pops out to me is that this patient has hyperopia. His foveal sensitivity is down a bit, and the right eye has two nasal depressed points. That may be nothing, but it’s something to keep in mind when you look at the optical coherence tomography (OCT).
Dr. Rhee: Dr. Piltz-Seymour, when you see the two points on Figure 1, how much weight do you put in the glaucoma Hemifield tests (GHT)? It might be a little hard to see on the Figure, but the test says it’s within normal limits despite the presence of two dark spots. How do you read this?
 Figure 1. Case 1: Baseline visual field.
Figure 1. Case 1: Baseline visual field.Jody Piltz-Seymour, MD: It’s curious that two adjacent points at the horizontal meridian are depressed. In conjunction with the depressed foveal threshold noted by Dr. Radcliffe, this might represent a very early glaucomatous visual field damage and needs to be correlated with the OCT.
Dr. Rhee: Dr. Sheybani, do you see anything striking about the OCT depicted in Figure 2?
 Figure 2. Case 1: Baseline OCT.
Figure 2. Case 1: Baseline OCT.Arsham Sheybani, MD: The nerves look of symmetric size, but when you have characteristic retinal nerve fiber layer (RNFL) asymmetry, especially inferiorly on that right eye, I start getting concerned. Glaucoma is characteristically an optic nerve disease that doesn’t necessarily involve pressure in the definition.1
Dr. Rhee: Is this glaucoma? Why or why not?
Dr. Radcliffe: Yes, it’s glaucoma because of two reasons in the right eye: the structure-function relationship and the characteristic optic neuropathy with a classic inferotemporal-bundle defect.
Dr. Rhee: I’m going to push on that. The GHT says it’s within normal limits. You’re still going to call that a visual field change?
Dr. Radcliffe: Yes, because mild glaucoma has a normal visual field. Once the GHT reads as abnormal, the patient has moderate glaucoma. We need to treat early, and we need to treat based on the optic nerve. The good news is we have OCT, which helps all of us diagnose glaucoma early. Don’t let a normal visual field test throw away a glaucoma diagnosis.
Dr. Sheybani: It can be difficult to give a diagnosis with upmost certainty right away; it requires time, especially if their pressures upon presentation are normal. I’d tell this patient that there is a high chance it is glaucoma given the appearance of the optic nerve.
Dr. Piltz-Seymour: I’d tell the patient that they most likely have glaucoma but that we have some time to gather information. They will most likely need therapy, but we have time to learn more about their baseline pressures and pressure variability. I’d also like to point out on the OCT depicted in Figure 2 that even though we see an inferior defect, the superior nerve fiber layer is also decreased compared with the other eye. This is most likely glaucoma, but there’s no reason to rush into treatment.
Dr. Rhee: What glaucoma therapy would you recommend for this patient in the first-line setting?
Dr. Radcliffe: I would recommend SLT.
Dr. Rhee: We often talk about SLT in the first-line setting at educational meetings, but what do you really do in the clinic? What percentage of patients do you start on SLT as a first-line therapy?
Dr. Radcliffe: SLT use has increased in my practice in the last decade. I’m privileged to treat patients who trust me and listen to what I recommend. When I have that dynamic with a patient, I always recommend SLT first.
Dr. Sheybani: I agree with Dr. Radcliffe; SLT is the clear choice. The LiGHT study enrolled 718 patients with treatment-naive POAG or ocular hypertension and randomly assigned them to SLT (n = 356) and drops (n = 362). At 36 months, 74% of SLT patients required no drops to maintain target IOP. They also had a lower rate of trabeculectomy. No patients in the SLT group needed a trabeculectomy, whereas 11 patients on medical management did.2 In the real world, however, the reality is that only 15 to 20% of patients will take me up on SLT at initial diagnosis.
Dr. Rhee: What about sustained-release treatments? Is there a role for it in initial therapy?
Dr. Piltz-Seymour: In this case, I don’t think so. This patient is young and will have this disease for a long time. Right now, the bimatoprost intracameral implant is the only sustained-release treatment approved for glaucoma and it is only approved as a single dose in each eye.3 I don’t think it is the right course for this patient. The LiGHT trial was a game-changer for me. Studies conducted prior to LiGHT also supported first-line SLT, but none with the power of the LiGHT trial.4 In this patient specifically, we also need to consider that his pressures are in the teens with normal CCT. This is normal-pressure glaucoma. We know from the Collaborative Normal Tension Glaucoma Study that lowering IOP by 30% in normal-tension glaucoma significantly decreased the risk of progression. However, we need to balance this with the fact that 40% of patients’ disease did not worsen over 5 or more years.5 It’s all about risk/benefit balance. So yes, this is most likely normal-tension glaucoma and yes, this patient will likely need IOP-lowering therapy, but you have some time to gather the information you need to learn about this patient’s IOP variability prior to offering treatment. Given the LiGHT trial results, SLT is an excellent first therapy as is topical therapy.
Dr. Sheybani: To be fair, it’s quite possible that this patient will have 6 to 10 mm Hg swings in pressure throughout the day. If you bring this patient back on a different day, at a different time, their pressure may be much higher.
Dr. Rhee: Would you still say this patient has glaucoma if the visual field showed a defect even after you repeated it, but the OCT was normal?
Dr. Piltz-Seymour: Yes, I would. The Ocular Hypertension Treatment Study (OHTS) showed that one-third of first defects were just in the visual field.6,7 You can have visual field loss with a normal OCT.
Dr. Sheybani: You did say that the visual field defect was repeatable in this case example, but it is worth noting that in OHTS, a large percentage of the initial abnormal visual fields were normal when they did them again. I still think I would weigh a lot on that function, because there’s a lot that OCT can miss, depending on the optic nerve and the way the papillary bundle is shaped.
Dr. Radcliffe: I need the OCT to give me some corroboration with the visual field. There are too many bad test takers out there. I’d like to spare them the side effects of therapy unless it’s absolutely necessary.
ROUND 1 |CASE 2: PROGRESSION ON OCT BUT NOT VISUAL FIELD WITH TARGET IOP
Dr. Rhee: Our second case is a 56-year-old self-identified woman of Asian ancestry who was referred for glaucoma treatment consultation for possible progression. Her VA is 20/20 OD and 20/25 OS. She is on latanoprost, which has been her only treatment at this point. Her current IOP is 19 mm Hg and 18 mm Hg in the right and left eyes, respectively, but the pressure maximums were 21 mm Hg and 20 mm Hg. There hasn’t been much IOP reduction with treatment. Her CCT is 525 µm and 520 µm. They are a little bit thin, but it’s not too bad. Her angles are a little bit shallow at D25. Figure 3 shows her visual fields and OCT. I want to highlight the circle on Figure 3, which show the change in the OCT. Is this progression? Is this change actionable?


 Figure 3. Case 2: Visual field and OCT follow-up over time.
Figure 3. Case 2: Visual field and OCT follow-up over time.Dr. Piltz-Seymour: It looks like there may be a little vitreomacular traction in the 2017 scan that’s gone in the 2018 scan. What looks like progression between the two scans may just be a result of release of the vitreomacular traction.
Dr. Radcliffe: I agree; there’s a little apparent thinning on the superior bundle, but it’s gone now. I think that may have been a tilted disc where in June 2018, the superotemporal fibers fell outside the OCT collection window, cutting them off. Remember that Spectralis flattens out the raw acquired OCT data on all nerves, aligning to a flat retinal pigment epithelium and masking optic nerve tilting and the collection window artifacts that go along with them. This is a tilted disc with some clipping of the superotemporal RNFL in the follow-up image.
Dr. Sheybani: I think Dr. Piltz-Seymour and Dr. Radcliffe have nailed it. We need to remember that depending on the study a large proportion of initial OCT scans can be affected by the vitreous base, whether it’s a posterior vitreous detachment or something causing vitreomacular traction or an opacity causing a signal obstruction. This is classic for me for this myopic patient. There is a very real chance that the RNFL in this region is normal, but it’s a split bundle. I would love a ganglion cell layer analysis of this patient.
Dr. Rhee: Let’s go back to their IOP. They started at 21 and 20 mm Hg and are now 19 and 18 mm Hg on latanoprost. Is that therapeutic?
Dr. Sheybani: To me, this patient is a nonresponder or isn’t taking the medicine.
Dr. Rhee: What is your next move? The patient is already on a prostaglandin analogue (PGA). Our options are medication, SLT, or sustained-release implant.
Dr. Piltz-Seymour: Does this patient have glaucoma? The only thing we have seen that is calling this glaucoma was the OCT. They have suspicious optic nerves. They have full fields. They may just have myopic nerves. I don’t know if it’s been proven to me that the patient has glaucoma. If the patient has glaucoma, this is a subtherapeutic treatment.
Dr. Rhee: Let me confirm that the patient has a strong family history of blindness at a relatively early age and the asymmetry that’s hinted here is real. What is your escalation therapy?
Dr. Piltz-Seymour: I think we have two excellent first options. One is SLT and the other is adding a Rho-associated protein kinase (ROCK) inhibitor like netarsudil. I think these are both excellent options to get the most bang for your buck with a single additional treatment.
Dr. Rhee: Dr. Sheybani, please talk a little bit about the complimentary mechanism of action (MOA) of latanoprost and netarsudil and SLT.
Dr. Sheybani: PGAs increase uveoscleral outflow.8 There is some outflow through the trabecular meshwork-based route. With ROCK inhibitors, there’s decreased resistance in the trabecular meshwork, cytoskeletal restructuring, but there’s also dilation. That’s why patients on ROCK inhibitors experience hyperemia. SLT is closer to the ROCK mechanism on the trabecular meshwork side of things where there is some remodeling there.9-11 When you’re thinking through the MOA of additive treatment, a lot of us would say adding a carbonic anhydrase inhibitor to a PGA has some effect.12 For this patient, I’d consider switching within the class if you want to stay dedicated to your PGA or remove it completely and see if there’s another medicine that is more effective.
Dr. Rhee: Dr. Radcliffe, what would you recommend for this patient?
Dr. Radcliffe: Assuming I tried to push them toward SLT and that wasn’t productive, I will switch within the class. However, switching within class means something new to me now. Whereas traditionally, I might say anything other than generic latanoprost is worth a try, we have new options now, including latanoprostene bunod with a nitric oxide mechanism. Nitric oxide improves the permeability of the trabecular meshwork to reduce IOP, and latanoprost acid targets the uveoscleral pathway.13-15 It’s two powerful medications in one bottle with a fixed combination of latanoprost and netarsudil. If the patient is tolerating latanoprost well and isn’t prone to hyperemia, I would escalate them in that manner. In glaucoma, particularly when there’s a question of progression, it’s good to be as definitive as possible or else they will continue to progress slowly.
Dr. Piltz-Seymour: When thinking about the next step, we must also consider adherence. What can we offer the patient that may better control their IOP, but that she will realistically use? The fewer times a medicine is dosed daily and the fewer bottles she has, the more likely she will continue treatment.16-19 That’s why combination netarsudil/latanoprost is a great switch here from latanoprost because of its strong IOP lowering with a single drop dosed once a day at bedtime.
Dr. Rhee: Excellent points. For the sake of argument, let’s say this patient is experiencing true progression. Her pressure is 14 mm Hg down from a max of 20 or 21 mm Hg. The patient insists she adheres with her medication. What do you do now?
Dr. Radcliffe: I’d explore the adherence issue a bit more, asking, for example, if she runs out of drops at the end of the month. That tends to happen to people who spill drops or who have trouble with coordination because you never get more than a month supply at once. I push hard not to believe that someone is really getting worse at 14 mm Hg because that puts them into a trabeculectomy space. I shoot for the low teens at all times, but I don’t shoot for the low single digits. That’s the dilemma here. I would bolster therapy for progression, ideally in a way that supports adherence.
Dr. Sheybani: Patients can experience great pressure variability. But if their pressure is truly 14 mm Hg and they are still progressing, I’d add drops. I don’t see many patients who need single-digit IOPs, but this person may be one of them. If they are progressing at 14 mm Hg, their target IOP should be 10 mm Hg or lower.
Dr. Piltz-Seymour: I would still add netarsudil, either as an addition or a switch to fixed-combination netarsudil/latanoprost because of the effect it can have on the episcleral venous pressure. Every now and then you have patients who come in with pressures in the high single digits, which you don’t see with other medicines. We know that netarsudil lowers pressure more consistently across a range of IOPs.20,21 I’m not saying that’s going to be the endgame for this patient, however. With a pressure of 14 mm Hg, you worry about other risk factors. Are they on too many blood pressure medicines? Are they having nocturnal hypotension?
ROUND 1 | CASE 3: FAILED SLT IN EARLY GLAUCOMA
Dr. Rhee: Our next case is a 74-year-old self-identified woman of African ancestry presenting after a failed SLT treatment performed in her left eye only 6 weeks ago. It didn’t work. The patient has a VA of 20/30 OU with medium glare. Her IOP and CCT is 21 mm Hg and 540 µm OD; 23 mm Hg and 550 µm OS. The slit lamp exam revealed 1+ NS and slightly narrow angle. This patient is on what many would consider as maximum therapy: latanoprost OU at bedtime; dorzolamide/timolol OU BID; and brimonidine 0.2% OU BID. Figure 4 shows her visual field and optic nerve scans.
 Figure 4. Case 3: Visual field and optic nerve scans.
Figure 4. Case 3: Visual field and optic nerve scans.Dr. Rhee: As a reminder, pressure is 21 and 23 mm Hg on latanoprost, dorzolamide/timolol, and brimonidine, and SLT had no effect in her left eye.
What are your next steps? Do you try SLT in her right eye? Do you add more medication? Do you recommend surgery? You can’t do a mix here because of the cataract.
Dr. Radcliffe: The patient has 8+ diopters of correction on that visual field and 4 D or 5 D of hyperopia. That tells me the cataracts aren’t going to last forever. I think SLTs deserve a 3-month window of efficacy. In my practice, I prefer to do both eyes before I check either for effect, because if you do it one way and wait for the effect, you’re assuming that the effect on the second eye is dependent on the success of the first. That is not the case.2 You’re better off lasering both eyes and giving them 6 weeks to 3 months, not giving up on the therapy for 3 months.
Dr. Sheybani: I think it’s reasonable to laser the other eye. In the LiGHT trial, if the SLT failed in the first eye, the second eye still received SLT, and they saw an effect.2 I think a conversation with the patient about lasering the second eye is reasonable. However, in this case specifically, the patient has paracentral loss, which is advanced disease. I would be very concerned that they won’t hit target IOP with either laser or medical management. I would move them to surgery.
Dr. Piltz-Seymour: This patient is on the road to surgery. You can try a branded medicine. You could change latanoprost to fixed-combination netarsudil/latanoprost, but the odds are that this person will need surgery.
Dr. Rhee: I’m going to raise the bar. What if their IOP was now 27 and 28 mm Hg? Would you consider the SLT effective? Do you still want to wait 3 months to evaluate efficacy?
Dr. Piltz-Seymour: I would go right to surgery.
Dr. Sheybani: I would also take them to surgery, but it’s a question of which kind. The cataract with a VA of 20/30 does not scare me. With a pressure of 27 and 28 mm Hg, almost regardless of what we do, we’re going to get a drop. I’d rather have a pressure in the low teens for this case. I think phacoemulsification or a 180° goniotomy is a reasonable approach for this patient.
Dr. Radcliffe: I would recommend phaco-MIGS for this patient, like the Xen Gel Stent (Allergan). I want to leave the eye as pristine as possible because cataract removal will be beneficial. Xen makes a lot of sense if you need 15 mm Hg of pressure reduction, which the Xen is capable of.22
Dr. Rhee: Dr. Sheybani, I’m going to hold you to the fact that the cataract cannot be removed. I agree that combined cataract-MIGS is a great option, but that is not on the table. What do you do instead?
Dr. Sheybani: Given the paracentral field loss, I’d give them the option between Xen or a primary tube. I would not do trabeculectomy when you have a pressure >22 mm Hg. Data from the Primary Tube Versus Trabeculectomy Study Group found that patients with IOP >22 mm Hg did better with the tube compared with trabeculectomy.23 That, plus the fact that this patient is African American and is at a higher risk for scarring, are why I would choose either Xen or primary tube.
Dr. Rhee: Why wouldn’t you do a trabeculectomy?
Dr. Sheybani: The Xen offers a lot of safety.22,24,25 Patients at a high risk of scarring still do well with it.
Dr. Piltz-Seymour: I’m still an avid trabeculectomy surgeon. I think that this patient would benefit most from a trabeculectomy in that left eye. Xen or trabeculectomy are reasonable options for that right eye. That said, I think you’re going to get the most consistent long-term pressure lowering from surgery. You can minimize the risk of side effects with excellent surgical technique and a consistent surgical procedure.
ROUND 1 |CASE 4: FAILED MIGS IN MODERATE TO ADVANCED GLAUCOMA
Dr. Rhee: Our next case is a 72-year-old woman of African ancestry. Her VA is 20/50 OU and her IOP is 24 mm Hg OD and 21 mm Hg OS. Her CCT is 515 µm OD and 512 µm OS. Her slit lamp exam shows 2 to 3 NS trace cortical changes. She’s on 5 medications (latanoprost, brimonidine/timolol, dorzolamide, and netarsudil), and had an SLT OU 6 months ago. Although the initial response to the SLT was good, her IOP has been slowly rising. Figure 5 shows her visual fields, which are impressive. What are you next steps for this patient? Would you do a trabeculectomy, cataract with MIGS, or something else?
 Figure 5. Case 4: Baseline visual field.
Figure 5. Case 4: Baseline visual field.Dr. Radcliffe: These are the cases I struggle with the most because we have such good treatments for the trabecular meshwork. It’s hard for me to leave them untouched, even when you have a case like this. This person needs tailored therapy. I’d talk to them and get a sense of their risk tolerance. If we were to do cataract surgery or some angle procedure, the patient must understand that they may need a follow-up surgery fairly quickly. You can do MIGS with a primary tube and a cataract and have a little bit of everything. That’s where I would head.
Dr. Piltz-Seymour: For me, this patient needs a trabeculectomy. They have very advanced glaucoma and significant cataract. Combined cataract-trabeculectomy unfairly gets bad press but is the perfect surgery for this person.26 People talk about doing trabeculectomy first, then cataract, but you may lose some bleb effectiveness from subsequent cataract extraction, and you still may need a bleb needling; that would be three potential surgeries. If you perform combined cataract-trabeculectomy first and it doesn’t work, you can still do the bleb needling, for a total of two potential surgeries. Combined cataract-trabeculectomy in this patient with diffuse application of injected mitomycin C will get you where you want to go fastest and let the patient get back on track with her life. It will give you the most direct route to low pressure and visual recovery.
Dr. Sheybani: This is a difficult case. For me, because her pressure is 24 mm Hg and the patient is of African ancestry, I would recommend phacoemulsification and a nonvalved tube. You have to warn them of potential complications. The part of their vision that they have is paracentral, but their inferior field is what has a little bit of function. This is where they will notice a difference if they lose visual field after a surgical complication.
Dr. Piltz-Seymour: Dr. Sheybani, what are you going to do in the period of time when that tube hasn’t opened?
Dr. Sheybani: That’s a valid point, but the same thing could happen with the trabeculectomy. We don’t know how the pressure may respond after you increase flow with suture adjustment in a trabeculectomy. Their pressure is 24 mm Hg with potentially two fenestrations. You know you have a good anterior chamber depth at the time of the surgery, and I feel reasonably comfortable that we’ll be able to ride through that issue. There are a couple of techniques you can do in the office to increase the chance of success. For example, 4 weeks out, I can laser suture lyse. You can add an oral carbonic anhydrase inhibitor. We can also adjust the tubes in the postoperative period.
Dr. Rhee: The patient underwent a cataract plus ab interno stent, and it did not work well enough. The IOP improved to 20 mm Hg on no medications, but the IOP is not at target. What medication would you add back first? Do you add a PGA or a ROCK inhibitor?
Dr. Piltz-Seymour: I would add back whatever will work and whatever the patient will take. I’d start with a PGA. I’d probably add a ROCK inhibitor, but if there are side effects, I’d go to other medicines. If a patient is on once-daily medication, the adherence is exponentially better than multidrug therapy.
Dr. Sheybani: I’d talk to the patient and ask her which medicine she'd like to restart. Some patients prefer a twice-daily dose. I’d rather start her on a PGA personally.
Dr. Radcliffe: I’d also ask the patient which drop she prefers. This is a chance to rebuild therapy. If she is on a generic drop and her insurance has changed, maybe you can pick a drop that she tolerates better. Often it’s a PGA that makes the most sense. Anything she's liked in the past, however, is a winner.
Dr. Rhee: Time continues and IOP control worsens. The patient underwent combined cataract and ab interno stent, which improved her IOP to 20 mm Hg. She is back on all medications and has now developed follicular conjunctivitis. She undergoes a trabeculectomy (Figure 6). HerVA is 20/20, and her IOP is 17 mm Hg. What medication do you add back first after the filtration procedure?
 Figure 6. Case 4: Bleb post-filtration surgery.
Figure 6. Case 4: Bleb post-filtration surgery.Dr. Sheybani: I would go with whatever the patient wants to start next. In all cases relative to the bleb, they are suppressing aqueous flow. If you’re worried about collapse of your bleb, all of them can do it, if you decrease the amount of flow that goes through there.
Dr. Piltz-Seymour: I like outflow more than aqueous suppressants. I think aqueous has many good characteristics for the eye. I would go with the PGA.
Dr. Rhee: At 3 months post-trabeculectomy her IOP is 3 mm Hg and VA is 20/50 (Figure 7). There’s not a lot of wiggle room with optic nerve health. What do you want to do from here?

 Figure 7. Case 4: Imaging 3 months post-trabeculectomy.
Figure 7. Case 4: Imaging 3 months post-trabeculectomy.Dr. Sheybani: Part of the discussion should be with the patient, because there is a chance that her peripheral vision could be maintained. The trabeculectomy is close to working. The first thing I’d do is go in with a needle and try to nick a scleral vessel and cause a hemorrhage, similar to an autologous blood injection, and see if I can focally wall that side off. If that doesn’t work, I’d try compression or Palmberg suture. I am not in favor of shutting down the bleb and then putting a tube shunt because I’m not sure it will be watertight.
Dr. Piltz-Seymour: The patient clearly has hypotony maculopathy. The question is, does she notice it? If she doesn't notice it, her eye is formed; I would leave it alone because of her advanced disease. It’s better to have 20/50 VA long-term than blindness. If she is noticing visual decline, I would take the patient back to the OR, and I’d irrigate the anterior chamber with trypan blue to see where the bleb is filtering. Even though there’s a big bleb, filtration usually only comes through the trabeculotomy flap in one little spot. I’d find out where that spot is and put in a transconjunctival suture, which is reversible. In a worst-case scenario if you get a leak, you can still do a bleb revision.
ROUND 2 | CASE 5: ACUTE ANGLE CLOSURE AFTER LASER IRIDOTOMY
Dr. Rhee: Our next case deals with acute angle closure after laser iridotomy. We’re joined by Dr. Piltz-Seymour; Thomas D. Patrianakos, DO; and JoAnn Giaconi, MD, to discuss this one. The patient is a 55-year-old woman of Asian ancestry with +2.75 D of hyperopia. She has a history of migraines, for which she takes propranolol for prophylaxis, but otherwise is in good health. She had laser iridotomies in 2015 for narrow angles. Vision at that time was 20/20 OU, and her pressures are usually around 15 mm Hg. When pressure in the right eye increased to 23 mm Hg she was started on latanoprost. The chart recorded bilateral laser iridotomies that transilluminated. Anterior chamber was narrow on Van Herick, lens had mild cataract, and a C/D of 0.4 and 0.2. She then moved and was followed by a local doctor.
She now presents urgently with pain, redness, and blurred vision. VA is now 20/400 OD and 20/20 OS. IOP is 42 mm Hg OD and 18 mm Hg OS. Slit lamp exam showed iris bombe OD with 1+ microcystic edema and shallow anterior chamber OD. Both laser peripheral iridotomies transilluminated. Gonioscopy was deferred OD because of the bombe and microcystic corneal edema. Gonioscopy in the left eye revealed appositional closure that opened with compression.
On further questioning, the patient describes that her migraines have worsened. There were no fortification spectra, but she had did have intermittent halos around light. The headaches were not pounding in nature and did not increase when she bent over or when she was exposed to loud noises or bright lights. The headaches diminished if she closed her eyes and meditated for about 10 to 20 minutes. What is going on here?
Thomas D. Patrianakos, DO: These are classic signs of acute angle closure.
JoAnn Giaconi, MD: I agree.
Dr. Rhee: This case is confusing, and I think there’s a teaching moment to be made here. What in this case could lead us astray?
Dr. Giaconi: Transillumination does not equal patency. So, you want to really look for patency of the peripheral iridotomy.
Dr. Rhee: How do you look for patency?
Dr. Piltz-Seymour: If you look directly at the laser iridotomy, you need to see a black hole; you need to see through the iris. Unfortunately, many doctors still use transillumination as a measure of patency. As Dr. Giaconi mentioned, transillumination is worthless in terms of assessing patency of an iridotomy. I tell residents that when you see people with pigmentary dispersion syndrome, they have transillumination defects all over the place, but these transillumination defects are not iridotomies. I hope we can convince people not to use transillumination to assess the patency of iridotomies. You need to look through the hole.
Dr. Patrianakos: One thing I’d like to add is if you have a patient with angle closure and you do a laser iridotomy, don’t just let them go. Many of these patients will require IOP-lowering medications, and some will still require surgery to reach target IOP.
Dr. Rhee: How would you know that this is not Posner-Schlossman syndrome?
Dr. Giaconi: Posner-Schlossman is glaucoma where people get very, very high pressures intermittently, but there’s no pupillary block mechanism in it. So, you would not expect to see the iris in bombe.
ROUND 3 |CASE 6: NEXT STEPS FOR A PATIENT INTOLERANT OF GENERIC PGA
Dr. Rhee: For our next case, we are joined by Dr. Patrianakos; Sameh Mosaed, MD; and Leon W. Herndon Jr, MD. This is a 61-year-old man of African ancestry. He took oral prednisone for 7 weeks and was diagnosed with glaucoma with a pressure maximum of 36 mm Hg and 42 mm Hg. He was started on latanoprost and dorzolamide/timolol. He did not tolerate dorzolamide/timolol, so he self-discontinued, and was only on latanoprost. However, he experienced intense burning and irritation from the latanoprost. His VA and CCT are 20/25 and 562 µm OD and 20/30 and 566 µm OS. Slit lamp exam shows early cataract 1+ NS and 1 to 2+ conjunctival hyperemia. Gonioscopy reveals open angles. Figure 8 shows his testing. On the OCT you can see some inferior loss. Now what? His IOP is not great, and he’s uncomfortable even with just one generic PGA at night. What are your options? Do you advise this person to continue with latanoprost or switch to a preservative-free option? Do you add or substitute for SLT? Try a sustained-release implant?

 Figure 8. Case 6: Baseline OCT and visual field.
Figure 8. Case 6: Baseline OCT and visual field.Dr. Patrianakos: SLT works well for a steroid-induced glaucoma. He probably has a combination of both steroid-induced and open-angle glaucoma. SLT would probably take care of the open-angle component and any steroid component of the elevated pressure. My first choice is an SLT, but we could also use the sustained-release bimatoprost implant.
Leon W. Herndon Jr, MD: All options you presented are reasonable. Certainly, this patient could be followed, but he’s not tolerating generic latanoprost very well. SLT could be considered, but to me, SLT doesn’t get patients off drops, so he would still need to use a topical medication. I would switch him to a preservative-free option.
Sameh Mosaed, MD: I would switch to a preservative-free drop and add SLT if the patient is willing to do it. You have to partner with the patient and listen to what they are willing to do. I don’t think this is steroid-induced glaucoma; I think it’s POAG being unmasked by the steroid use. A sustained-release implant is a temporary fix, and glaucoma is a lifelong disease. I don’t see a role for a temporary fix in a lifelong process. That said, SLT is also temporary, but you get more out of it with fewer side effects.
Dr. Rhee: Just to tell you what I did, I switched the latanoprost to preservative-free tafluprost and added preservative-free dorzolamide/timolol. One month later, the pressure was 14 mm Hg and he was tolerating the drops well.
ROUND 3 | CASE 7: WELL-CONTROLLED IOP BUT GLARE AND DIFFICULTY READING ON MULTIDRUG REGIMEN
Dr. Rhee: Our final case is a 75-year-old woman of Latin ancestry who complains of glare with oncoming headlights and difficulty reading. Her VA is 20/50 OU. Her IOP is 9 mm Hg OD and 10 mm Hg OS, so it’s well controlled. However, she has thin corneas (512 µm OD and 516 µm OS). Optic nerve is 0.9 OU. She is on latanoprost, dorzolamide/timolol, and netarsudil. She is intolerant to both generic and branded brimonidine. She has moderate to severe visual field loss, but four central points around fixation are not involved. The patient wants cataract surgery. What would you do?
Dr. Patrianakos: I would cautiously offer her cataract surgery, and then discuss with her the various options to take her off some of those medications. I would offer some type of MIGS to reduce her medication burden. The complex regimen is likely making her life miserable and could be causing some of the glare and reading difficulty. While we’re in there removing the cataract, we could also do a goniotomy or trabeculotomy. The goal isn’t to lower the pressure—I don’t think we’re going to get much better pressure—but his could help reduce her drops. I would probably do a combination trabeculotomy goniotomy.
Dr. Herndon: I think a combination cataract and glaucoma procedure would be reasonable. I think for MIGS, we still need to go subconjunctival. I’d combine the cataract surgery with the Xen to shunt fluid from the anterior chamber to the subconjunctival space. With the Xen by external approach, there are fewer cases of needling, and it provides pretty good control. That doesn’t preclude doing more surgery in the future, but it’s the most effective MIGS procedure we have right now.
Dr. Mosaed: This is a difficult decision because I think all the options are good. However, I wouldn’t do a subconjunctival procedure because when combined with cataract surgery there is more inflammation and a greater risk of scarring. The failure rate is a bit higher. I want to salvage the real estate and be able to do something with that later if necessary. I would do an ab interno MIGS and pair that with the cataract extraction. I prefer nonimplant MIGS because they all achieve fairly similar outcomes, but nonimplant procedures avoid short- and long-term implant-related complications. I’d prefer to do one without leaving an implant in the eye, so I would do a goniotomy.
Dr. Rhee: This was a well-controlled patient on four medications. You could do cataract surgery, you could do combined cataract and MIGS. I did cataract surgery with the Hydrus Microstent (Alcon). When I performed the surgery, it wasn’t flush up against the trabecular meshwork; it stuck out. This is something that can happen. What do you do? Would you leave it in place and see how the patient does or remove it?
Dr. Herndon: If it’s not in the right place the patient will have some discomfort during the procedure. I don’t think we leave it there as is. A poorly placed device is not good for the patient long term. I would retrieve it and try again.
Dr. Rhee: That concludes our case discussion of personalized treatment plans for glaucoma management. I appreciate all the panelists sharing their wisdom and expertise.
1. Gedde SJ, Vinod K, Wright MM, et al. Primary open-angle glaucoma preferred practice pattern®. Ophthalmology. 2021;128(1):P71-P150.
2. Gazzard G, Konstantakopoulou E, Garway-Heath D, et al. Selective laser trabeculoplasty versus eye drops for first-line treatment of ocular hypertension and glaucoma (LiGHT): a multicentre randomised controlled trial [published correction appears in Lancet. 2019;394(10192):e1]. Lancet. 2019;393(10180):1505-1516.
3. Allergan. Durysta Prescribing Information. https://media.allergan.com/products/durysta_pi.pdf. Revised November 2020. Accessed May 5, 2022.
4. Chi SC, Kang YN, Hwang DK, Liu CJ. Selective laser trabeculoplasty versus medication for open-angle glaucoma: systematic review and meta-analysis of randomised clinical trials. Br J Ophthalmol. 2020;104(11):1500-1507.
5. Anderson DR; Normal Tension Glaucoma Study. Collaborative normal tension glaucoma study. Curr Opin Ophthalmol. 2003;14(2):86-90.
6. Kass MA, Heuer DK, Higginbotham EJ, et al. The ocular hypertension treatment study: a randomized trial determines that topical ocular hypotensive medication delays or prevents the onset of primary open-angle glaucoma. Arch Ophthalmol. 2002;120(6):701-830.
7. Gordon MO, Kass MA. What we have learned from the ocular hypertension treatment study. Am J Ophthalmol. 2018;189:xxiv-xxvii.
8. Toris CB, Gabelt BT, Kaufman PL. Update on the mechanism of action of topical prostaglandins for intraocular pressure reduction. Surv Ophthalmol. 2008;53 Suppl1:S107-S120.
9. Kazemi A, McLaren JW, Kopczynski CC, Heah TG, Novack GD, Sit AJ. The effects of netarsudil ophthalmic solution on aqueous humor dynamics in a randomized study in humans. J Ocul Pharmacol Ther. 2018;34(5):380-386.
10. Sit AJ, Gupta D, Kazemi A, et al. Netarsudil improves trabecular outflow facility in patients with primary open angle glaucoma or ocular hypertension: a phase 2 study. Am J Ophthalmol. 2021;226:262-269.
11. Asrani S, Bacharach J, Holland E, et al. Fixed-dose combination of netarsudil and latanoprost in ocular hypertension and open-angle glaucoma: pooled efficacy/safety analysis of phase 3 MERCURY-1 and -2. Adv Ther. 2020;37(4):1620-1631.
12. Stoner A, Harris A, Oddone F, et al. Topical carbonic anhydrase inhibitors and glaucoma in 2021: where do we stand? [published online ahead of print, 2021 Aug 25]. Br J Ophthalmol. 2021;bjophthalmol-2021-319530.
13. Mehran NA, Sinha S, Razeghinejad R. New glaucoma medications: latanoprostene bunod, netarsudil, and fixed combination netarsudil-latanoprost. Eye (Lond). 2020;34(1):72-88.
14. Cavet ME, Vittitow JL, Impagnatiello F, Ongini E, Bastia E. Nitric oxide (NO): an emerging target for the treatment of glaucoma. Invest Ophthalmol Vis Sci. 2014;55(8):5005-5015.
15. Lee AJ, McCluskey P. Clinical utility and differential effects of prostaglandin analogs in the management of raised intraocular pressure and ocular hypertension. Clin Ophthalmol. 2010;4:741-764.
16. Robin A, Grover DS. Compliance and adherence in glaucoma management. Indian J Ophthalmol. 2011;59 Suppl(Suppl1):S93-S96.
17. Babić N. Fixed Combinations of Glaucoma Medications. Srp Arh Celok Lek. 2015;143(9-10):626-631.
18. Tapply I, Broadway DC. Improving adherence to topical medication in patients with glaucoma. Patient Prefer Adherence. 2021;15:1477-1489.
19. Gatwood J, Brooks C, Meacham R, et al. Facilitators and barriers to glaucoma medication adherence. J Glaucoma. 2022;31(1):31-36.
20. Zaman F, Gieser SC, Schwartz GF, Swan C, Williams JM. A multicenter, open-label study of netarsudil for the reduction of elevated intraocular pressure in patients with open-angle glaucoma or ocular hypertension in a real-world setting. Curr Med Res Opin. 2021;37(6):1011-1020.
21. Peace JH, McKee HJ, Kopczynski CC. A randomized, phase 2 study of 24-h efficacy and tolerability of netarsudil in ocular hypertension and open-angle glaucoma. Ophthalmol Ther. 2021;10(1):89-100.
22. Fea AM, Durr GM, Marolo P, Malinverni L, Economou MA, Ahmed I. XEN gel stent: a comprehensive review on its use as a treatment option for refractory glaucoma. Clin Ophthalmol. 2020;14:1805-1832.
23. Gedde SJ, Feuer WJ, Lim KS, et al. Treatment outcomes in the primary tube versus trabeculectomy study after 3 years of follow-up. Ophthalmology. 2020;127(3):333-345.
24. Reitsamer H, Vera V, Ruben S, et al. Three-year effectiveness and safety of the XEN gel stent as a solo procedure or in combination with phacoemulsification in open-angle glaucoma: a multicentre study. Acta Ophthalmol. 2022;100(1):e233-e245.
25. Wagner FM, Schuster AK, Emmerich J, Chronopoulos P, Hoffmann EM. Efficacy and safety of XEN-implantation vs. trabeculectomy: data of a “real-world” setting. PLoS One. 2020;15(4):e0231614.
26. Davila JR, Singh K, Hernandez-Boussard T, Wang S. Outcomes of primary trabeculectomy versus combined phacoemulsification-trabeculectomy using automated electronic health record data extraction [published online ahead of print, 2022 Mar 23]. Curr Eye Res. 2022;1-7.